Table of Contents
About This Issue
Severe traumatic brain injury (TBI) is a time-critical emergency, and early decisions made in the ED can influence neurologic recovery and survival. Optimal patient outcomes depend on rapid recognition, close attention to oxygenation and perfusion, timely identification of life-threatening associated injuries, and evidence-based management of elevated intracranial pressure. This issue reviews current best practices for the evaluation and stabilization of patients with severe TBI and addresses ongoing controversies in acute management. In this issue, you will learn:
Key priorities in the initial assessment and resuscitation of patients with severe TBI
How to identify concomitant diagnoses that may worsen outcomes, including nontraumatic precipitating factors
Strategies for maintaining adequate cerebral perfusion and preventing hypotension
Indications for neuroimaging and how imaging findings guide management
Evidence-based approaches to the recognition and tier-based treatment of elevated intracranial pressure
Criteria for neurosurgical consultation and appropriate patient disposition
Current controversies regarding hyperosmolar therapy, tranexamic acid, and other interventions
- About This Issue
- Abstract
- Case Presentations
- Introduction
- Critical Appraisal of Literature
- Pathophysiology, Epidemiology, and Etiology
- Pathophysiology
- Subarachnoid Hemorrhage
- Epidural Hematoma
- Subdural Hematoma
- Contusions
- Diffuse Axonal Injury
- Epidemiology
- Etiology
- Classification of Traumatic Brain Injury
- Clinical Classification
- Mechanistic Classification
- Radiographic Classification
- Differential Diagnosis
- Prehospital Care
- Emergency Department Evaluation
- History
- Physical Examination
- Diagnostic Studies
- Imaging Studies
- Computed Tomography
- Ultrasonography
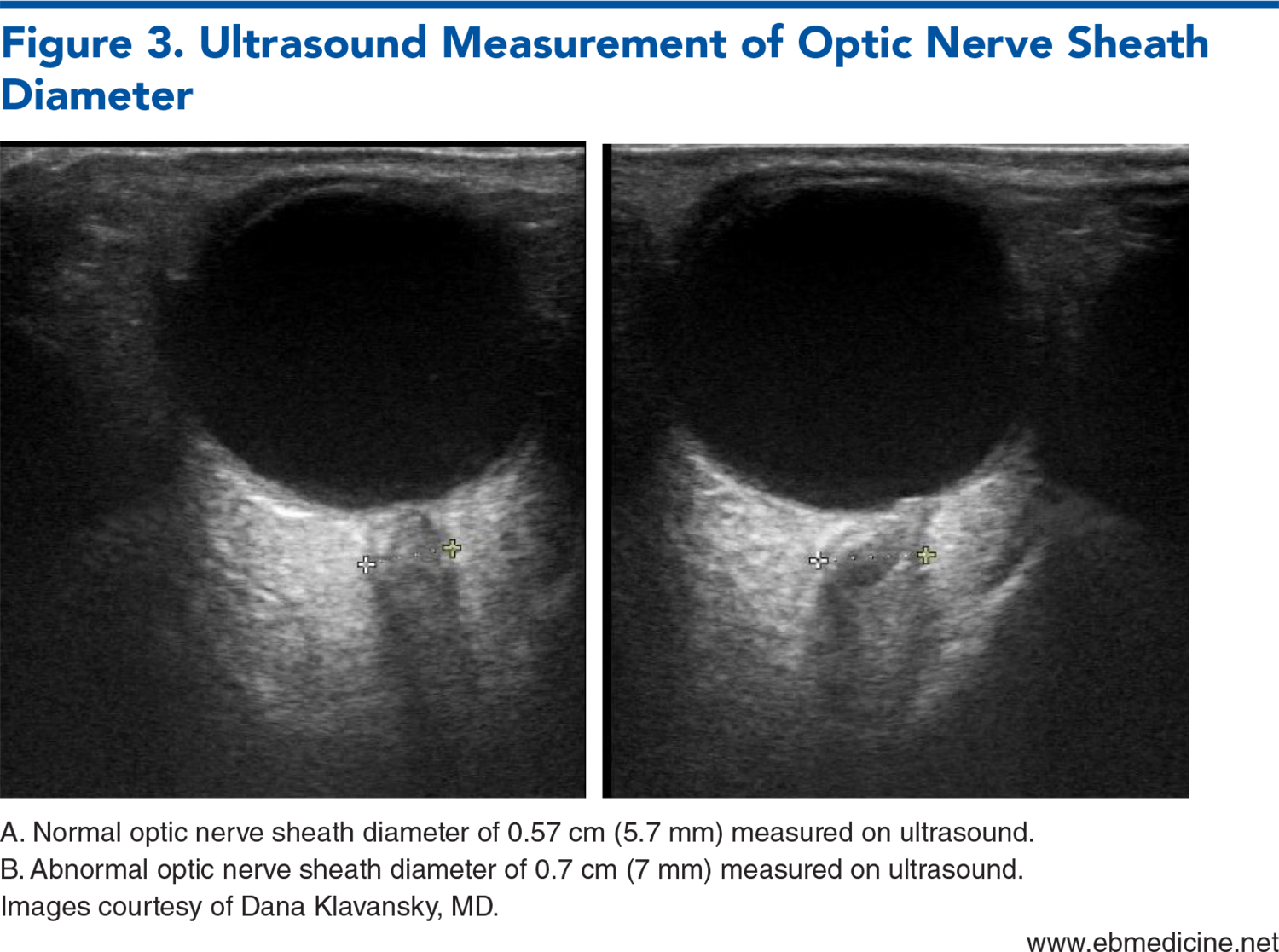
- Optic Nerve Sheath Diameter
- Optic Disc Elevation
- Other Imaging Modalities
- Pupillometry
- Fluid Biomarkers
- Neuron-Specific Enolase
- Ubiquitin Carboxy-Terminal Hydrolase L1
- S100 Calcium-Binding Protein B
- Tau
- Treatment
- Initial Stabilization and Management
- Airway Management
- Rapid Sequence Intubation
- Ventilation Strategies
- Hyperosmolar Therapy
- Cerebral Perfusion and Hemodynamic Management
- Temperature and Metabolic Management
- Coagulopathies and Reversal
- Prevention of Infectious Complications
- Prophylaxis for Deep Vein Thrombosis
- Management of Cerebral Venous Sinus Thrombosis
- Management of Posttraumatic Seizures
- Management of Intracranial Hypertension
- Intracranial Pressure Monitoring
- Tiered Approach to Management of Elevated Intracranial Pressure
- Surgical Management
- Prognosis and Outcome Prediction
- Special Circumstances
- Repeat Head Injuries
- Second Impact Syndrome
- Chronic Traumatic Encephalopathy
- Combat-Related Traumatic Brain Injury
- Controversies and Cutting Edge
- Multimodal Prognostication
- Tranexamic Acid
- Disposition
- 5 Things That Will Change Your Practice
- Risk Management Pitfalls for Emergency Department Management of Severe Traumatic Brain Injury
- Summary
- Time and Cost-Effective Strategies
- Case Conclusions
- Clinical Pathway for Management of Patients With Suspected Severe Traumatic Brain Injury
- Tables and Figures
- References
Abstract
Traumatic brain injury is a significant cause of long-term disability and death worldwide. Recent advances in the acute management of traumatic brain injury have improved outcomes across the full spectrum of disease, including severe injury. Early recognition, optimization of oxygenation and perfusion, and appropriate disposition are essential components of care for patients with severe traumatic brain injury. A systematic history and physical examination are critical to identifying life-threatening injuries and guiding timely interventions, including management of elevated intracranial pressure. This review summarizes current evidence-based recommendations for the emergency department evaluation and management of severe traumatic brain injury, highlights ongoing controversies, and identifies key areas for future research.
Case Presentations
- He reports that the headache began after he sustained a head injury in an assault, but is unable to provide any additional details.
- He says he takes aspirin at home.
- A noncontrast CT of the head shows an acute 0.5-cm right temporal subdural hemorrhage.
- Should you consult neurosurgery for emergent surgical intervention? What medical interventions are indicated? Should repeat imaging be obtained, and if so, when?
- EMS reports that she was not wearing a helmet when the crash occurred.
- Her GCS score on arrival at the ED is 6. You immediately place a cervical collar and intubate the patient to stabilize her for imaging.
- A noncontrast CT of the head shows a 0.6-cm right subdural hematoma with 0.7-cm leftward midline shift, subarachnoid hemorrhage in the suprasellar cistern, a 0.2-cm epidural hematoma, and a nondisplaced skull fracture.
- Is additional imaging indicated? What initial interventions should you consider?
- EMS reports that the patient was mumbling incoherently and had a GCS score of 12 at the scene.
- On arrival at the ED, his GCS score is 10. He is no longer verbal but does appear to be protecting his airway.
- A noncontrast CT of the head shows a left temporal depressed skull fracture, additional frontal and parietal fractures, left lateral and medial orbital wall fracture, a 0.7-cm subdural hemorrhage, a 0.2-cm epidural hemorrhage, and a 3-mm rightward midline shift of the brain, with a small left parietal intraparenchymal hemorrhage.
- What are your immediate treatment options, and what neurosurgical interventions are indicated?
How would you manage these patients? Subscribe for evidence-based best practices and to discover the outcomes.
Clinical Pathway for Management of Patients With Suspected Severe Traumatic Brain Injury
Subscribe to access the complete Clinical Pathway to guide your clinical decision making.
Tables and Figures
Subscribe for full access to all Tables and Figures.
Buy this issue and
CME test to get 4 CME credits.
Key References
Following are the most informative references cited in this paper, as determined by the authors.
5. * Meyfroidt G, Bouzat P, Casaer MP, et al. Management of moderate to severe traumatic brain injury: an update for the intensivist. Intensive Care Med. 2022;48(6):649-666. (Review) DOI: 10.1007/s00134-022-06702-4
8. * Carney N, Totten AM, O'Reilly C, et al. Guidelines for the management of severe traumatic brain injury, fourth edition. Neurosurgery. 2017;80(1):6-15. (Brain Trauma Foundation consensus guidelines) DOI: 10.1227/NEU.0000000000001432
10. * Lulla A, Lumba-Brown A, Totten AM, et al. Prehospital guidelines for the management of traumatic brain injury - 3rd edition. Prehosp Emerg Care. 2023;27(5):507-538. (Brain Trauma Foundation consensus guidelines for prehospital providers) DOI: 10.1080/10903127.2023.2187905
17. * Marehbian J, Muehlschlegel S, Edlow BL, et al. Medical management of the severe traumatic brain injury patient. Neurocrit Care. 2017;27(3):430-446. (Review) DOI: 10.1007/s12028-017-0408-5
25. * Manley GT, Dams-O'Connor K, Alosco ML, et al. A new characterisation of acute traumatic brain injury: the NIH-NINDS TBI classification and nomenclature initiative. Lancet Neurol. 2025;24(6):512-523. (Proposed study framework) DOI: 10.1016/S1474-4422(25)00154-1
35. * Gravesteijn BY, Sewalt CA, Stocchetti N, et al. Prehospital management of traumatic brain injury across europe: a CENTER-TBI study. Prehosp Emerg Care. 2021;25(5):629-643. (Multicenter observational cohort study; 3878 patients) DOI: 10.1080/10903127.2020.1817210
91. * Vrettou CS, Mentzelopoulos SD. Second- and third-tier therapies for severe traumatic brain injury. J Clin Med. 2022;11(16):4790. (Review)
92. * Patel S, Maria-Rios J, Parikh A, et al. Diagnosis and management of elevated intracranial pressure in the emergency department. Int J Emerg Med. 2023;16(1):72. (Review) DOI: 10.1186/s12245-023-00540-x
96. * Muehlschlegel S, Rajajee V, Wartenberg KE, et al. Guidelines for neuroprognostication in critically ill adults with moderate-severe traumatic brain injury. Neurocrit Care. 2024;40(2):448-476. (Clinical practice guideline) DOI: 10.1007/s12028-023-01902-2
97. * Nasrallah F, Bellapart J, Walsham J, et al. PREdiction and Diagnosis using Imaging and Clinical biomarkers Trial in Traumatic Brain Injury (PREDICT-TBI) study protocol: an observational, prospective, multicentre cohort study for the prediction of outcome in moderate-to-severe TBI. BMJ Open. 2023;13(4):e067740. (Observational prospective cohort study protocol) DOI: 10.1136/bmjopen-2022-067740
Subscribe to get the full list of 102 references and see how the authors distilled all of the evidence into a concise, clinically relevant, practical resource.
Keywords: TBI, severe, traumatic, intracranial, hemorrhage, pressure, ICP, CPP, EDH, SDH, SAH, herniation, hematoma, intraparenchymal, GCS, midline, CT, MRI, coagulopathy, cerebral perfusion, blood pressure, intubation, hyperosmolar