Table of Contents
-
Abstract
-
Case Presentations
-
Introduction
-
Critical Appraisal Of The Literature
-
Epidemiology And Etiology
-
Lower Gastrointestinal Bleeding
-
Intussusception
-
Pathophysiology
-
Lower Gastrointestinal Bleeding
-
Risk Factors For Lower Gastrointestinal Bleeding
-
Intussusception
-
Risk Factors For Intussusception
-
Differential Diagnosis
-
Lower Gastrointestinal Bleeding
-
Intussusception
-
Prehospital Treatment
-
Emergency Department Evaluation
-
History
-
Physical Examination
-
Intussusception
-
Diagnostic Studies
-
Laboratory Tests
-
Lower Gastrointestinal Bleeding Imaging Studies
-
Intussusception Imaging Studies
-
Treatment
-
Lower Gastrointestinal Bleeding
-
Intussusception
-
Special Circumstances
-
Controversies And Cutting Edge
-
Disposition
-
Summary
-
Risk Management Pitfalls For Lower Gastrointestinal Bleeding
-
Case Conclusion
-
Tables and Figures
-
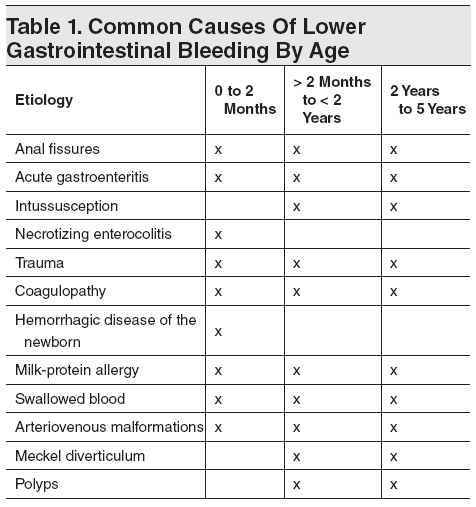
Table 1. Common Causes Of Lower Gastrointestinal Bleeding By Age
-
Table 2. Risk Factors For Lower Gastrointestinal Bleeding
-
Table 3. Common Imaging Modalities In Lower Gastrointestinal Bleeding And Intussusception
-
Figure 1. Sample Discharge Instruction
-
References
Abstract
Lower gastrointestinal (LGI) bleeding in the pediatric patient 5 years of age or younger is an uncommon ED presentation that causes anxiety and concern both in the child’s family and in the clinician. A report from Boston Children’s Hospital in the early 1990s showed that rectal bleeding was a presenting complaint in 0.3% of pediatric patients who visited the emergency department (ED) within a 1-year period. The emergency clinician may find this presentation daunting, since the differential diagnosis of LGI bleeding includes numerous age-specific disorders not found in the adult population, ranging from self-limited anal fissures to surgical emergencies. The time to diagnosis and reduction will influence morbidity and mortality in these patients; hence, the emergency clinician should have a high index of suspicion as well as knowledge of current evidence for diagnosis and treatment. This issue of Pediatric Emergency Medicine Practice reviews the common differential diagnoses of LGI bleeding in children younger than 5 years of age, relying on the best available evidence from the literature. Readers will be able to apply clinically appropriate guidelines regarding diagnosis and treatment in an effective and patient-specific manner. In particular, this article focuses on the challenge of evaluating and managing the pediatric patient with intussusception.
Case Presentations
A 3-year-old female presents to your ED with the chief complaint of diffuse abdominal pain and nonbloody, nonbilious vomiting over the past 2 days. Her mother tells you that, after vomiting, the child becomes “lethargic and lies still in pain.” These events are self-limited, lasting a few minutes. The patient is otherwise healthy and has been afebrile without diarrhea. On physical examination, the child appears well and is interactive but is somewhat listless. She has no fever and, except for a heart rate of up to 115 beats per minute, her vital signs are within normal limits. Auscultation of her abdomen indicates normo-active bowel sounds. Her abdomen is soft and distended, with mild diffuse tenderness. A fecal occult blood test comes back positive. Her intermittent abdominal pain raises your suspicion for possible intussusception, which is suggested by the presence of occult blood in the stool. With many imaging modalities available, as well as consultants on hand, you suspect you’ll be able to confirm or confidently rule out this diagnosis.
Introduction
The possibility of bleeding from the LGI tract in a young child causes anxiety for the child’s family. The general emergency clinician may find this presentation daunting, since the differential diagnosis of LGI bleeding includes numerous age-specific disorders not found in the adult population. Many emergency clinicians do not feel comfortable discharging the pediatric patient with recent LGI bleeding, and disposition can present a challenge. By assessing for age-specific pathologies and obtaining a thorough clinical history and examination, the emergency clinician will narrow diagnostic choices, thereby optimizing management and further care of the pediatric patient with LGI bleeding.
This issue of Pediatric Emergency Medicine Practice will review the common differential diagnoses of LGI bleeding in children younger than 5 years of age, relying on the best available evidence from the literature. In particular, it will focus on the challenge of evaluating and managing the pediatric patient with intussusception. The emergency clinician will be able to apply clinically appropriate guidelines regarding diagnosis and treatment in an effective and patient-specific manner.
Critical Appraisal Of The Literature
A large number of articles have been published regarding outcomes in patients with intussusception who were treated with various modalities; specifically, hydrostatic and pneumostatic reduction and surgery. Much of this research involved retrospective cohort studies. This review focuses on these findings in detail.
An extensive search of the literature on pediatric LGI bleeding and intussusception between 1970 and 2011 using Ovid MEDLINE® and PubMed was conducted. Keywords included pediatric GI bleeding, intussusception, Meckel diverticulum, bowel malrotation, milk-protein sensitivity, milk-protein allergy, pediatric GI hemorrhage, blood per rectum, inflammatory bowel disease, necrotizing enterocolitis, GI arteriovenous malformation, and pediatric rectal/anal trauma. The search was limited to studies involving persons between 0 and 18 years of age.
Risk Management Pitfalls For Lower Gastrointestinal Bleeding
-
“The 6-month-old patient had a vague history of colicky abdominal pain, but he appeared well in the ED. This looked like a milk-protein allergy.”
Intussusception classically presents with colicky abdominal pain, and the patient may appear well between painful episodes. A positive fecal occult blood test can support a suspicion of intussusception, although it may also be positive in the child with milk-protein allergy. History is an important tool in narrowing the differential diagnosis. Milk-protein allergy is not likely to begin acutely in this older patient. Ultrasound should be used to diagnose intussusception. Observation in the ED may also be warranted if ultrasound is unavailable, and it may be helpful in deciding whether to obtain a CT scan, which would expose the patient to radiation.
-
“The 10-year-old patient had colicky abdominal pain, but she was too old to have intussusception.”
Although intussusception is most common in younger patients, it can occur at any age. The incidence of intussusception associated with a pathologic lead point increases with age.
-
“Intussusception in the 3-year-old patient was successfully reduced, and though she appeared well, I decided to admit her for observation, since 50% of recurrences occur in the first 48 hours.”
Hospital admission is not indicated in the easily and successfully reduced case of idiopathic intussusception if, after a period of observation in the ED, the patient returns to baseline status and tolerates oral intake without vomiting or pain. Hospital admission to monitor for recurrence after a simple reduction in the well-appearing patient is not warranted and imposes significant costs on the healthcare system. Family counseling must be given, as well as clear discharge instructions regarding returning to the ED in the event of abdominal pain, vomiting, or bloody stools.
-
“The patient had frank hematochezia, but it didn’t resemble redcurrant jelly stools, so intussusception was lower on my differential.”
Although it is considered the “classic” presentation, intussusception does not commonly present with redcurrant jelly stools. Frank hematochezia is a presenting sign in about 60% of cases of intussusception.
-
“Though this patient appeared well, the stools were grossly bloody, which warranted an in-depth work-up.”
Many food products and medications may give the false appearance of bloody stools. The presence of blood should be confirmed with a fecal occult blood test prior to initiating further evaluation in the stable patient.
-
“I thought my patient had intussusception, but her abdomen was tender and it was more efficient to obtain a CT scan to rule out other possible GI pathologies, like appendicitis.”
Ultrasonography is a sensitive and specific imaging modality for intussusception. If available, an ultrasound examination will spare the patient exposure to the radiation from a CT scan. If the ultrasound result is negative or inconclusive, CT would be the next option.
-
“It was the middle of the night and the ultrasound technician wouldn’t be available for another 4 hours. Although I thought the patient had intussusception, he appeared well, so I waited until the tech arrived.”
Ultrasonography is the best imaging choice for diagnosing intussusception and will avoid unnecessary radiation exposure from CT. However, a delay in diagnosis and therapeutic reduction can increase the risk for complications. If ultrasound is unavailable and you suspect intussusception, a CT scan should be obtained.
Tables and Figures
References
Evidence-based medicine requires a critical appraisal of the literature based upon study methodology and number of subjects. Not all references are equally robust. The findings of a large, prospective, randomized, and blinded trial should carry more weight than a case report.
To help the reader judge the strength of each reference, pertinent information about the study, such as the type of study and the number of patients in the study, will be included in bold type following the reference, where available. In addition, the most informative references cited in this paper, as determined by the authors, will be noted by an asterisk (*) next to the number of the reference.
-
* Teach SJ, Fleisher GR. Rectal bleeding in the pediatric emergency department. Ann Emerg Med. 1994;23:1252-1258. (Retrospective case series; 104 children)
-
Stav K, Reif S. Gastrointestinal bleeding in children--etiology and diagnosis. Survey of patients in a Tel Aviv medical center, in the years 1990 to 1997. Harefuah. 2000;138:534-538, 615. (Retrospective case series; 201 children)
-
Torres AM, Ziegler MM. Malrotation of the intestine. World J Surg. 1993;17:326-331. (Retrospective case series; 22 children)
-
Andrassy RJ, Mahour GH. Malrotation of the midgut in infants and children. Arch Surg. 1981;116:158-160. (Retrospective case series; 74 children)
-
Yimyaem P, Chongsrisawat V, Vivatvakin B, et al. Gastrointestinal manifestations of cow’s milk protein allergy during the first year of life. J Med Assoc Thai. 2003;86:116-123. (Retrospective case series; 10 children)
-
Hirose R, Yamada T, Hayashida Y. Massive bloody stools in two neonates caused by cow’s milk allergy. Pediatr Surg Int. 2006;22:935-938. (Case study; 2 patients)
-
Piccoli D. Colitis. eMedicine.com. June 4th 2010. http://emedicine.medscape.com/article/927845-overview. Last viewed December 13, 2011.
-
Nocerino A. Protein intolerance. eMedicine.com. April 12th, 2010. http://emedicine.medscape.com/article/931548-overview. Last viewed December 13, 2011.
-
Sugar NF, Feldman KW. Perineal impalements in children: distinguishing accident from abuse. Pediatr Emerg Care. 2007;23:605-616. (Retrospective case series; 34 cases)
-
Frank JD, Brown S. Thermometers and rectal perforations in the neonate. Arch Dis Child. 1978;53:824-825. (Case series; 3 neonates)
-
Christensen RD, Pysher TJ, Christensen SS. Case report: perianal necrotizing fasciitis in a near-term neonate. J Perinatol. 2007;27:390-391. (Case study)
-
Heyman MB, Kirschner BS, Gold BD, et al. Children with early-onset inflammatory bowel disease (IBD): analysis of a pediatric IBD consortium registry. J Pediatr. 2005;146:35-40. (Retrospective cohort; 1370 patients)
-
Malaty HM, Fan X, Opekun AR, et al. Rising incidence of inflammatory bowel disease among children: a 12-year study. J Pediatr Gastroenterol Nutr. 2010;50:27-31. (Retrospective cohort; 272 children)
-
Baumgart DC, Sandborn WJ. Inflammatory bowel disease: clinical aspects and established and evolving therapies. Lancet. 2007;369:1627-1657.
-
* Parashar UD, Holman RC, Cummings KC, et al. Trends in intussusception-associated hospitalizations and deaths among US infants. Pediatrics. 2000;106:1413-1421. (Retrospective cohort; discharge data review)
-
Blanch A, Perel S, Acworth J. Paediatric intussusception: epidemiology and outcome. Emerg Med Australas. 2007;19:45-50. (Review)
-
Awasthi S, Agarwal G, Mishra V, et al. Four-country surveillance of intestinal intussusception and diarrhea in children. J Paediatr Child Health. 2009;45:82-86. (Prospective surveillance study; 2519 patients)
-
* DiFiore JW. Intussusception. Semin Pediatr Surg. 1999;8:214-220. (Systematic review)
-
* Stringer MD, Pablot SM, Brereton RJ. Paediatric intussusception. Br J Surg. 1992;79:867-876. (Systematic review)
-
Lloyd DA, Kenny SE. The surgical abdomen. In: Walker WA, Goulet O, Kleinman RE, et al, eds. Pediatric Gastrointestinal Disease: Pathopsychology, Diagnosis, Management. 4th ed. Ontario, Canada: Mosby; 2004:604. (Textbook)
-
Tseng YC, Lee MS, Chang YJ, et al. Acute abdomen in pediatric patients admitted to the pediatric emergency department. Pediatr Neonatol. 2008;49:126-134. (Retrospective case series; 400 patients)
-
Kaiser AD, Applegate KE, Ladd AP. Current success in the treatment of intussusception in children. Surgery. 2007;142:469-475; discussion 475-477. (Review)
-
Leonidas JC. Treatment of intussusception with small bowel obstruction: application of decision analysis. AJR Am J Roentgenol. 1985;145:665-669. (Decision analysis)
-
Gierup J, Jorulf H, Livaditis A. Management of intussusception in infants and children: a survey based on 288 consecutive cases. Pediatrics. 1972;50:535-546. (Case series; 288 patients)
-
Spalding SC, Evans B. Intussusception. Emerg Med. 2004;36:12-19. (Review)
-
Blanco, FC. Intussusception. eMedicine.com. July 19th, 2011. http://eMedicine.medscape.com/article/802424-overview. Last viewed December 13, 2011.
-
* Navarro O, Daneman, A. Intussusception. Part 3: diagnosis and management of those with an identifiable or predisposing cause and those that reduce spontaneously. Pediatr Radiol. 2004;34:305-312. (Systematic review)
-
Pang LC. Intussusception revisited: clinicopathologic analysis of 261 cases, with emphasis on pathogenesis. South Med J. 1989;82:215-228. (Case series; 261 patients)
-
Turunen S, Karttunen TJ, Kokkonen J. Lymphoid nodular hyperplasia and cow’s milk hypersensitivity in children with chronic constipation. J Pediatr. 2004;145:606-611. (Case control; 50 patients)
-
* Blakelock, RT, Beasley, SW. The clinical implications of non-idiopathic intussusception. Pediatr Surg Int. 1998;14:163-167. (Systematic review)
-
Kliegman RM, Behrman RE, Jenson HB, et al. Nelson Textbook of Pediatrics. 18th ed. Philadelphia, Pa: Saunders Elsevier; 2007. (Textbook)
-
* Bajaj L, Roback M. Postreduction management of intussusception in a children’s hospital emergency department. Pediatrics. 2003;112:1302-1307. (Retrospective cohort; 123 children)
-
Shalkow J. Small bowel obstruction. eMedicine.com. November 8, 2011. http://eMedicine.medscape.com/article/930411-overview. Last viewed December 13, 2011.
-
Yamamoto LG, Morita SY, Boychuk RB, et al. Stool appearance in intussusception: assessing the value of the term “currant jelly.” Am J Emerg Med. 1997;15:293-298. (Retrospective cohort; 107 patients)
-
Khuroo MS. Ascariasis. Gastroenterol Clin North Am. 1996;25:553-577. (Systematic review)
-
Zanardi LR, Haber P, Mootrey GT, et al. Intussusception among recipients of rotavirus vaccine: reports to the vaccine adverse event reporting system. Pediatrics. 2001;107:E97. (Retrospective case series; 98 patients)
-
Murphy TV, Gargiullo PM, Massoudi MS, et al. Intussusception among infants given an oral rotavirus vaccine. N Engl J Med. 2001;344:564-572. (Retrospective case control; 2192 patients)
-
Kramarz P, France EK, Destefano F, et al. Population-based study of rotavirus vaccination and intussusception. Pediatr Infect Dis J. 2001;20410-416. (Cohort; 56,253 patients)
-
Vesikari T, Matson DO, Dennehy P, et al. Safety and efficacy of a pentavalent human-bovine (WC3) reassortant rotavirus vaccine. N Engl J Med. 2006;354:23-33. (Randomized control trial; 2066)
-
Choong CK, Beasley SW. Intra-abdominal manifestations of Henoch-Schönlein purpura. J Paediatr Child Health. 1998;34:405-409. (Review)
-
Holmes M, Murphy V, Taylor M, et al. Intussusception in cystic fibrosis. Arch Dis Child. 1991;66:726-727. (Review)
-
St-Vil D, Brandt ML, Panic S, et al. Meckel’s diverticulum in children: a 20-year review. J Pediatr Surg. 1991;26:1289-1292. (Review)
-
Karpac CA, Li X, Terrell DR, et al. Sporadic bloody diarrhoea-associated thrombotic thrombocytopenic purpura-haemolytic uraemic syndrome: an adult and paediatric comparison. Br J Haematol. 2008;141:696-707. (Retrospective cohort; 6021)
-
Fox VL. Gastrointestinal bleeding in infancy and childhood. Gastroenterol Clin North Am. 2000;29:37-66,v. (Review)
-
Brown DL, Kouides PA. Diagnosis and treatment of inherited factor X deficiency. Haemophilia. 2008;14:1176-1182. (Review)
-
Gála I, Tòth L, Szegedi L, et al. Gastric bleeding in a patient with rheumatoid arthritis complicated by immune thrombocytopenic purpura. Joint Bone Spine. 2008;75:350-352. (Case report)
-
Reish O, Nachum E, Naor N, et al. Hemophilia B in a neonate: unusual early spontaneous gastrointestinal bleeding. Am J Perinatol. 1994;11:192-193. (Case report)
-
Ziemski JM, Szczepanik AB, Misiak A, et al. Endoscopic injection treatment of gastrointestinal bleeding in hemophiliacs. World J Surg. 1996;20:1166-1170. (Prospective cohort; 89 patients)
-
Forbes CD, Barr RD, Prentice CR, et al. Gastrointestinal bleeding in haemophilia. Q J Med. 1973;42:503–511. (Review)
-
Guillevin L, Le Thi Hound D, Godeau P, et al. Clinical findings and prognosis of polyarteritis nodosa and Churg-Strauss angiitis: A study of 165 patients. Br J Rheumatol. 1988;27:258-264. (Retrospective cohort; 165 patients)
-
Scott DG, Bacon PA, Elliott PJ, et al. Systemic vasculitis in a district general hospital 1972-1980: clinical and laboratory features, classification and prognosis of 80 cases. Q J Med. 1982;51:292-311.
-
Lopez LR, Schocket AL, Standford RE, et al. Gastrointestinal involvement in leukocytoclastic vasculitis and polyarteritis nodosa. J Rheumatol. 1980;7:677-684. (Retrospective case series; 80 patients)
-
Pagnoux C, Mahr A, Cohen P, et al. Presentation and outcome of gastrointestinal involvement in systemic necrotizing vasculitides: analysis of 62 patients with polyarteritis nodosa, microscopic polyangiitis, Wegener granulomatosis, Churg-Strauss syndrome, or rheumatoid arthritis-associated vasculitis. Medicine (Baltimore.) 2005;84:115-128. (Case series; 62 patients)
-
Meier DE, Coln CD, Rescorla FJ, et al. Intussusception in children: international perspective. World J Surg. 1996;20:1035-1039. (Review)
-
* Immordino PA. Intussusception in children: a review of 10 years’ experience in a community hospital. Conn Med. 1977;41:76-79. (Systematic review)
-
Bruce J, Huh YS, Cooney DR, et al.Intussusception: evolution of current management. J Pediatr Gastroenterol Nutr. 1987;6:663-674. (Systematic review)
-
Losek JD, Fiete RL. Intussusception and the diagnostic value of testing stool for occult blood. Am J Emerg Med. 1991;9:1-3. (Retrospective cohort; 96 children)
-
* Holtz L, Neill M, Tarr P. acute bloody diarrhea: a medical emergency for patients of all ages. Gastroenterology. 2009;136:1887-1898. (Systematic review)
-
* Silber G. Lower gastrointestinal bleeding. Pediatr Rev. 1990;12:85-93. (Systematic review)
-
Fleischer GR, Ludwig S, eds. Synopsis of Pediatric Emergency Medicine. 4th Ed. Lippincott, Williams and Wilkins. 2002:95. (Textbook)
-
Ralston M, Hazinski MF, Zaritsky AL, et al. Pediatric Advanced Life Support Provider Manual. Dallas,TX. American Heart Association Subcommittee on Pediatric Resuscitation; 2006:227-232. (Textbook)
-
Sheldon CA. The pediatric genitourinary examination. Inguinal, urethral, and genital diseases. Pediatr Clin North Am. 2001;48:1339-1380. (Review)
-
Odze RD, Wershil BK, Leichtner AM, et al. Allergic colitis in infants. J Pediatr. 1995;126:163-170. (Review)
-
del-Pozo G, Albillos JC, Tejedor D, et al. Intussusception in children: current concepts in diagnosis and enema reduction. Radiographics. 1999;19:299-319. (Systematic review)
-
Hryhorczuk AL, Strouse PJ. Validation of US as a first-line diagnostic test for assessment of pediatric ileocolic intussusception. Pediatr Radiol. 2009;39:1075-1079. (Retrospective cohort; 814 patients)
-
Rohrschneider W, Tröger J, Betsch B. The post-reduction donut sign. Pediatr Radiol. 1994;24:156-160. (Case series; 30 patients)
-
Sargent MA, Babyn P, Alton DJ. Plain abdominal radiography in suspected intussusception: a reassessment. Pediatr Radiol. 1994;24:17-20. (Cohort; 182 x-rays)
-
West KW, Stephens B, Vane DW, et al. Intussusception: current management in infants and children. Surgery. 1987;102:704-710. (Retrospective cohort; 83 patients)
-
Daneman A, Navarro O. Intussusception Part 2: An update on the evolution of management. Pediatr Radiol. 2004;34:97-108. (Review)
-
Hernanz-Schulman M, Foster C, Maxa R, et al. Experimental study of mortality and morbidity of contrast media and standardized fecal dose in the peritoneal cavity. Pediatr Radiol. 2000;30:369-378. (Case control; 100 animals)
-
Daneman A, Alton DJ, Ein S, et al. Perforation during attempted intussusception reduction in children: a comparison of perforation with barium and air. Pediatr Radiol. 1995;25:81-88. (Cohort; 14 children)
-
Krishnakumar, Hameed S, Umamaheshwari. Ultrasound guided hydrostatic reduction in the management of intussusception. Indian J Pediatr. 2006;73:217-220. (Case series; 25 patients)
-
Chan KL, Saing H, Peh WC, et al. Childhood intussusception: ultrasound-guided Hartmann’s solution hydrostatic reduction or barium enema reduction? J Pediatr Surg. 1997;32:3-6. (Case control; 46 patients)
-
Crystal P, Hertzanu Y, Farber B, et al. Sonographically guided hydrostatic reduction of intussusception in children. J Clin Ultrasound. 2002;30:343-348. (Retrospective case series; 83 patients)
-
Humphry A, Ein SH, Mok PM. Perforation of the intussuscepted colon. AJR Am J Roentgenol. 1981;137:1135-1138. (Retrospective case series; 850 patients)
-
Maoate K, Beasley SW. Perforation during gas reduction of intussusception. Pediatr Surg Int.1998;14:168-170. (Retrospective case series; 650 patients)
-
Guo JZ, Ma XY, Zhou QH. Results of air pressure enema reduction of intussusception: 6,396 cases in 13 years. J Peadiatr Surg. 1986;21:1201-1203. (Retrospective study, 6396 children)
-
Ko HS, Schenk JP, Tröger J, et al. Current radiological management of intussusception in children. Eur Radiol. 2007;17:2411-2421. (Systematic review)
-
* González-Spínola J, Del Pozo G, Tejedor D, et al. Intussusception: the accuracy of ultrasound-guided saline enema and the usefulness of a delayed attempt at reduction. J Pediatr Surg. 1999;34:1016-1020. (Cohort study; 195 children)
-
Alvarez-Caro F, Concha-Torre JA, García-Hernández I, et al. Massive lower gastrointestinal haemorrhage, successfully treated with corticosteroids, as main symptom of Schönlein-Henoch purpura. Rheumatol Int. 2009;29:1491-1494. (Case report)
-
Moustafa MH, Taylor M, Fletcher L. “My two-week-old daughter is throwing up blood.” Acad Emerg Med. 2005;12:775-777. (Case report)
-
Bonadio WA. Intussusception reduced by barium enema. Outcome and short term follow-up. Clin Pediatr (Phila). 1988;27:601-604. (Retrospective case review; 88 patients)
-
Eshel G, Barr J, Heiman E, et al. Incidence of recurrent intussusception following barium vs air enema. Acta Pediatr. 1997;86:545-546. (Retrospective case review; 97 patients)
-
Wolfram W. Pediatric gastrointestinal bleeding. eMedicine.com. March 29, 2011. http://eMedicine.medscape.com/article/940176-overview. Last viewed December 13, 2011.