Table of Contents
-
Abstract
-
Case Presentations
-
Critical Appraisal Of The Literature
-
Asthma Literature
-
Anticholinergics
-
Magnesium Sulfate
-
Theophylline
-
Ketamine
-
Bronchiolitis Literature
-
Beta-agonists
-
Epinephrine
-
Steroids
-
Apnea
-
Other Treatment Modalities
-
Croup Literature
-
Steroids
-
Cool Mist
-
Heliox
-
Foreign Body Aspiration Literature
-
Anaphylaxis Literature
-
Epidemiology
-
Pathophysiology
-
Etiology / Differential Diagnosis
-
Upper Airway Etiologies
-
Lower Airway Etiologies
-
Chest Wall / Pleural Cavity
-
Cardiac
-
Nervous System
-
Gastrointestinal
-
Metabolic
-
Prehospital Care
-
Emergency Department Evaluation
-
History
-
Timing
-
Preceding Symptoms
-
Type Of Cough
-
Vomiting
-
Past Medical History
-
Family History
-
Physical Examination
-
General Appearance And The Work Of Breathing
-
How fast?
-
How hard?
-
How loud?
-
Vital Signs
-
Head Examination
-
Neck Examination
-
Chest Examination
-
Abdominal Examination
-
Skin Examination
-
Neurological Examination
-
Diagnostic Studies
-
Radiology
-
Neck X-Rays
-
Blood Gases
-
Capnometry
-
Pulse Oximetry
-
Respiratory Syncytial Virus Testing
-
Treatment
-
Airway Management
-
Oxygen
-
Bag-Valve-Mask / Assisted Ventilation
-
Endotracheal Intubation
-
Alternative Airways
-
Surgical Airways
-
Foreign Body Removal
-
Pharmacologic Therapy
-
Bronchodilators
-
Vasoconstrictors
-
Anticholinergics
-
Steroids
-
Antibiotics
-
Special Circumstances
-
H1N1 Influenza
-
Cystic Fibrosis
-
Sickle Cell Anemia
-
Bronchopulmonary Dysplasia / Chronic Lung Disease
-
Immunosuppressed Children
-
Steroid Dependent Asthmatics
-
Neuromuscular Disorders
-
Controversies/Cutting Edge
-
Noninvasive Ventilation
-
Isomeric Albuterol
-
Helium Oxygen Mixture
-
Ketamine
-
Disposition
-
Summary
-
Clinical Pathway: Emergency Department Evaluation Of Infants/Toddlers With Respiratory Distress (Not Wheezing)
-
Clinical Pathway: Emergency Department Evaluation Of Wheezing Infants And Toddlers
-
Clinical Pathway: Emergency Department Approach to Infant/Child Difficulty Breathing
-
Risk Management Pitfalls In The Treatment Of Difficulty Breathing
-
Tables and Figures
-
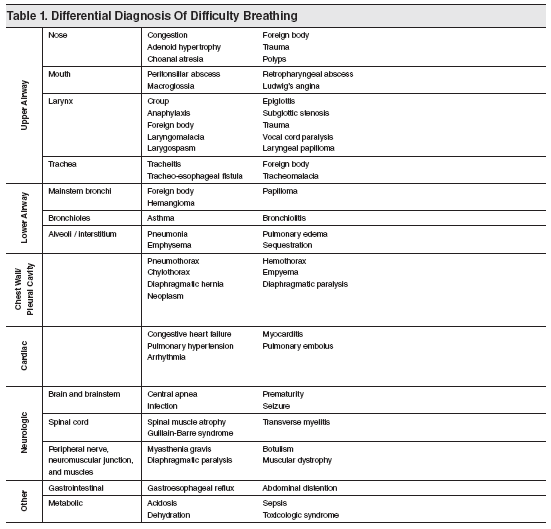
Table 1. Differential Diagnosis Of Difficulty Breathing Upper Airway
-
Table 2. Rapid Sequence Intubation
-
References
Abstract
Pediatric respiratory distress is a common and troubling presenting complaint to the emergency department (ED). Although many respiratory illnesses are due to upper respiratory tract infections, which are self-limited and need only parental reassurance, the emergency clinician must constantly be alert and prepared for the few children with an underlying condition that can progress to respiratory compromise or failure. Emergency clinicians must utilize clues from both the history and physical examination to uncover the cause of the distress and then employ the most up-to-date modalities to prevent the child’s deterioration. Although uncommon, respiratory failure can rapidly ensue in some instances and cause cardiopulmonary arrest. Respiratory failure is the most common cause of cardiac arrest in children.1 The unexpected and rapid respiratory collapse of the pediatric patient can most often be avoided by early recognition of the severity of illness and should prompt initiation of appropriate therapies.
Case Presentations
You’ve just come in for the early morning shift. You finish taking sign-outs. As you walk toward the coffee machine, the triage nurse runs by you carrying a toddler in her arms who is coughing, crying, and gasping for air. You follow her to the room, squeeze past 2 frightened parents, a crying grandparent, 2 other nurses, and an EMT student trying to get to the child. They are all trying to keep him on the gurney, place monitor leads, place a nasal cannula for oxygen, and start looking for IV sites. In the meantime, the child’s distress continues to worsen, and everyone in the room starts looking at you.
Critical Appraisal Of The Literature
Due to the number of conditions that result in respiratory distress, the literature on this topic is quite extensive and diverse. While certain illnesses are well-studied, the literature on other disease states is sparse. For instance, the scope of the literature on foreign body aspiration is limited to case reports and case series. This is due to the fact that there are only a handful of cases each year that present to a single ED, making it difficult to conduct large studies. On the other hand, there are many large randomized trials and systematic reviews on asthma, bronchiolitis, and croup.
Risk Management Pitfalls In The Treatment Of Difficulty Breathing
-
“It can’t be asthma – the child wasn’t wheezing.” Children with asthma who are very sick may present with a “silent chest” due to very poor air exchange. The severe degree of bronchoconstriction seen in these patients is thought to obstruct airflow sufficiently to impede wheezing. Many times, the initiation of beta-agonist therapy with albuterol will result in the patient manifesting wheezing.
-
“What do you mean he’s now apneic? His respiratory rate was normal just a little while ago!” As children progress from respiratory distress to respiratory fatigue, they will start to breathe more slowly. It can be dangerous to assume that a child who is breathing more slowly is clinically improving.
-
“Congestive heart failure!? The baby didn’t have rales.” Congestive heart failure in infants may not typically manifest with rales. Instead, assessing the presence of hepatomegaly on physical examination or noting a history of sweating during feeds will more likely identify cases of congestive heart failure in infants.
-
“It couldn’t be pertussis – the baby was not whooping.” Few infants with pertussis infection have the classis paroxysmal cough. Be suspicious of pertussis infection with a history of prolonged cough or apnea, in under-immunized infants.
-
“How could this be a foreign body – there was no history, and the chest x-ray was clear?” Often, a foreign body aspiration will not have an accompanying history, and a child will present with new onset wheezing (occasionally unilateral) without predisposing factors. A normal chest x-ray does not rule out a foreign body. A high index of suspicion is often necessary to make the diagnosis.
-
“The patient’s croup got better after the epinephrine treatment — so I sent her home.” Although the theoretical “rebound” effect of racemic epinephrine has not been substantiated in the literature, patients with croup and resting stridor require additional treatment and evaluation after the effects of the epinephrine have worn off.
Tables and Figures
References
Evidence-based medicine requires a critical appraisal of the literature based on study methodology and number of subjects. Not all references are equally robust. The findings of a large, prospective, randomized, and blinded trial should carry more weight than a case report.
To help the reader judge the strength of each reference, pertinent information about the study, such as the type of study and the number of patients in the study, will be included in bold type following the reference, where available.
-
Rotta AT, Wiryawan B. Respiratory emergencies in children. Respiratory Care. 2003;48(3):248-258; discussion 258-260. (Review)
-
Anonymous. NHLBI issues updated guidelines for the diagnosis and management of asthma. American Family Physician. 1997;56(2):621-623. (Guideline)
-
Ratto D, Alfaro C, Sipsey J, et al. Are intravenous corticosteroids required in status asthmaticus? JAMA. 1988;260(4):527-529. (Randomized prospective; 77)
-
Harrison BD, Stokes TC, Hart GJ, et al. Need for intravenous hydrocortisone in addition to oral prednisolone in patients admitted to hospital with severe asthma without ventilatory failure. Lancet. 1986;1(8474):181-184. (Double-blind, placebo-control; 52)
-
Becker JM, Arora A, Scarfone RJ, et al. Oral versus intravenous corticosteroids in children hospitalized with asthma. J Allergy Clin Immunol. 1999;103(4):586-590. (Double-blind,placebo-control; 66)
-
Barnett PL, Caputo GL, Baskin M, et al. Intravenous versus oral corticosteroids in the management of acute asthma in children. Ann Emerg Med. 1997;29(2):212-217. (Prospective randomized, controlled; 49)
-
Qureshi F, Zaritsky A, Poirier MP. Comparative efficacy of oral dexamethasone versus oral prednisone in acute pediatric asthma. J Pediatr. 2001;139(1):20-26. (Prospective, randomized; 533)
-
Hendeles L. Selecting a systemic corticosteroid for acute asthma in young children. Journal of Pediatrics, 2003;142(2 Suppl):S40-44. (Review)
-
Gries DM, Moffitt DR, Pulos E, et al. A single dose of intramuscularly administered dexamethasone acetate is as effective as oral prednisone to treat asthma exacerbations in young children. J Pediatr. 2000;136(3):298-303.(Prospective,randomized, blinded; 32)
-
Edmonds ML, Camargo CA, Pollack CV, et al. Early use of inhaled corticosteroids in the emergency department treatment of acute asthma.(update of Cochrane Database Syst Rev. 2001;(1)CD002308; PMID: 11279763). Cochrane Database of Syst. 2003(3):CD002308. (Systematic review)
-
Camargo CA, Rachelefsky G, Schatz M. Managing asthma exacerbations in the emergency department: summary of the National Asthma Education and Prevention Program Expert Panel Report 3 guidelines for the management of asthma exacerbations. J Allergy Clin Immunol. 2009;124(2 Suppl):S5-14. (Guideline)
-
Schuh S, Reisman J, Alsheri M, et al. A comparison of inhaled fluticasone and oral prednisone for children with severe acute asthma. New Engl Journ Med. 2000;343(10):689-694. (Prospective, randomized, controlled; 44)
-
Devidayal, Singhi S, Kumar L, et al. Efficacy of nebulized budesonide compared to oral prednisolone in acute bronchial asthma. Acta Paediatr. 1999;88(8):835-840. (Prospective,randomized, double-blind; 80)
-
Expert Panel Report 3 (EPR-3): Guidelines for the Diagnosis and Management of Asthma-Summary Report 2007. J Allergy Clin Immunol. 2007;120(5 Suppl):S94-138. (Guideline)
-
CatesCJ, Rowe BH, Bara A, Holding chambers versus nebulisers for beta-agonist treatment of acute asthma. Cochrane Database of Syst Rev. 2002(2):CD000052. (Systematic Review)
-
Schuh S, Johnson DW, Stephens D, Callahan S, et al. Comparison of albuterol delivered by a metered dose inhaler with spacer versus a nebulizer in children with mild acute asthma. J Pediatr. 1999. 135(1):22-27. (Randomized, doubleblind; 90)
-
Chou, KJ, Cunningham SJ, Crain EF. Metered-dose inhalers with spacers vs nebulizers for pediatric asthma. Arch Pediatr Adolesc Med. 1995;149(2):201-205. (Randomized; 152)
-
Castro-Rodriguez JA, Rodrigo GJ. beta-agonists through metered-dose inhaler with valved holding chamber versus nebulizer for acute exacerbation of wheezing or asthma in children under 5 years of age: a systematic review with meta-analysis. J Pediatr. 2004;145(2):172-177. (Systematic Review)
-
Ben-Zvi Z, Lam C, Hoffman J, Teets-Grimm KC, et al. An evaluation of the initial treatment of acute asthma. Pediatrics, 1982. 70(3):348-353. (Review)
-
Becker AB, Nelson NA, Simons FE. Inhaled salbutamol (albuterol) vs injected epinephrine in the treatment of acute asthma in children. J Pediatr. 1983;102(3):465-469. (Doubleblind; 40)
-
Qureshi F, Zaritsky A, Lakkis H. Efficacy of nebulized ipratropium in severely asthmatic children. Ann Emer Med. 1997;29(2):205-211. (Randomized, double-blind, placebocontrol; 90)
-
Cleary-Hammarstedt C, Flynn CA. Do children with acute asthma benefit more from anticholinergics and beta-2 agonists than from beta-2 agonists alone? Am Fam Physician. 2002;66(3):417-418. (Review)
-
Rodrigo G J, Castro-Rodriguez JA. Anticholinergics in the treatment of children and adults with acute asthma: a systematic review with meta-analysis. (erratum appears in Thorax. 2006;61(3):274. Thorax. 2005;60(9) 740-746. (Systematic review)
-
Craven D, Kercsmar, Myers TR, et al. Ipratropium bromide plus nebulized albuterol for the treatment of hospitalized children with acute asthma. J Pediatr. 2001;138(1):51-58. (Randomized, double-blind, placebo-control; 210)
-
Ciarallo L, Brousseau D, Reinert S. Higher-dose intravenous magnesium therapy for children with moderate to severe acute asthma. Arch Pediatr Adolesc Med. 2000. 154(10):979-983.(Prospective, randomized; 30)
-
Scarfone RJ, Loiselle JM, Joffe MD, et al. A randomized trial of magnesium in the emergency department treatment of children with asthma. Ann Emerg Med. 2000;36(6):572-578. (Prospective, randomized, controlled; 54)
-
Rowe BH, Bretzlaff JA, Bourdon C, et al. Magnesium sulfate for treating exacerbations of acute asthma in the emergency department. Cochrane Database Syst Rev. 2000(2):CD001490. (Systematic review)
-
Silverman RA, Osborn H, Runge J, et al. IV magnesium sulfate in the treatment of acute severe asthma: a multicenter randomized controlled trial. Erratum appears in Chest. 2002;122(5):1870. Chest. 2002;122(2):489-497. (Randomized, controlled, multi-center; 248)
-
Blitz M, Blitz S, Hughes R, et al. Aerosolized magnesium sulfate for acute asthma: a systematic review. Erratum appears in Chest. 2005;128(5)3779). Chest. 2005;128(1):337-344. (Systematic Review)
-
Kazaks AG, Uriu-Adams JY, Albertson TE, et al. Effect of oral magnesium supplementation on measures of airway resistance and subjective assessment of asthma control and quality of life in men and women with mild to moderate asthma: a randomized placebo controlled trial. J Asthma. 47(1):83-92. (Randomized, placebo-controlled; 55)
-
Ream RS, Loftis LL, Albers GM, et al. Efficacy of IV theophylline in children with severe status asthmaticus. Chest. 2001;119(5):1480-1488. (Systematic review)
-
Petrillo TM, Fortenberry JD, Linzer JF, et al. Emergency department use of ketamine in pediatric status asthmaticus. J Asthma. 2001;38(8):657-664. (Prospective; 10)
-
Howton, JC, Rose J, Duffy S, et al. Randomized, doubleblind, placebo-controlled trial of intravenous ketamine in acute asthma. Ann Emer Med. 1996;27(2):170-175. (Prospective, randomized, controlled; 54)
-
Rock, MJ, Reyes de la Rocha S, L’Hommedieu CS, et al. Use of ketamine in asthmatic children to treat respiratory failure refractory to conventional therapy. Crit Care Med. 1986;14(5):514-516. (Case-series; 2)
-
L’Hommedieu CS, Arens JJ. The use of ketamine for the emergency intubation of patients with status asthmaticus. Ann Emerg Med. 1987;16(5):568-571. (Case-series; 5)
-
Mallory MD, Shay DK, Garret J, et al. Bronchiolitis management preferences and the influence of pulse oximetry and respiratory rate on the decision to admit. Pediatrics. 2003;111(1:e45-51.(Survey; 519)
-
Brown L, Heterogeneity, evidence and salt. CJEM. 2004. 6(3)165-166. (Comment)
-
Kellner JD, Ohlsson A, Gadomski, et al. Efficacy of bronchodilator therapy in bronchiolitis. A meta-analysis. Arch Pediatr Adolesc Med. 1996;150(11):1166-1172. (Meta-analysis)
-
Flores G, Horwitz RI. Efficacy of beta2-agonists in bronchiolitis: a reappraisal and meta-analysis. Pediatrics. 1997;100(2 Pt 1):233-239. (Meta-analysis)
-
Hartling L, Wiebe N, Russell K, et al. A meta-analysis of randomized controlled trials evaluating the efficacy of epinephrine for the treatment of acute viral bronchiolitis. Arch Pediatr Adolesc Med. 2003;157(10):957-964. (Meta-analysis)
-
King VJ, Viswanathan M, Bordley WC, et al. Pharmacologic treatment of bronchiolitis in infants and children: a systematic review. Arch Pediatr Adolesc Med. 2004;158(2):127-137. (Systematic Review)
-
Gadomski AM, Bhasale AL. Bronchodilators for bronchiolitis. Cochrane Database Syst Rev. 2006;3:CD001266. (Systematic review)
-
AAP and S.o.D.a.M.o. Bronchiolitis, Diagnosis and management of bronchiolitis. Pediatrics. 2006. 118(4):1774-1793. (Guideline)
-
Patel H, Gouin S, Platt RW. Randomized, double-blind, placebo-controlled trial of oral albuterol in infants with mild-tomoderate acute viral bronchiolitis. J Pediatr. 2003.142(5):509-514. (Randomized, double-blind, placebo-control; 129)
-
Menon K, Sutcliffe T, Klassen TP. A randomized trial comparing the efficacy of epinephrine with salbutamol in the treatment of acute bronchiolitis. J Pediatr. 1995;126(6):1004-1007. (Randomized, controlled; 42)
-
Ralston S, Hartenberger C, Anaya T, et al. Randomized, placebo-controlled trial of albuterol and epinephrine at equipotent beta-2 agonist doses in acute bronchiolitis. Pediatr Pulmonol. 2005;40(4):292-299. (Randomized, double-blind, placebo-control; 65)
-
Wainwright C, Altamirano, Cheney M, et al. A multicenter, randomized, double-blind, controlled trial of nebulized epinephrine in infants with acute bronchiolitis. N Engl J Med. 2003;349(1):27-35. (Randomized, double-blind, controlled; 194)
-
van Woensel JB, Wolfs TF, van Aalderen WM, et al. Randomised double-blind placebo controlled trial of prednisolone in children admitted to hospital with respiratory syncytial virus bronchiolitis. Thorax. 1997;52(7):634-637. (Randomized, double-blind, controlled; 40)
-
Roosevelt G, Sheehan K, Grupp-Phelan J, et al. Dexamethasone in bronchiolitis: a randomised controlled trial. Lancet. 1996;348(9023):292-295. (Prospective, randomized, controlled, 118)
-
De Boeck K, Van der Aa N, Van Lierde S, et al. Respiratory syncytial virus bronchiolitis: a double-blind dexamethasone efficacy study. J Pediatr. 1997;131(6):919-921. (Prospective, randomized, controlled; 29)
-
Klassen TP, Sutcliffe T, Watters LK, et al. Dexamethasone in salbutamol-treated inpatients with acute bronchiolitis: a randomized, controlled trial. J Pediatr. 1997. 130(2):191-6. (Randomized, controlled; 61)
-
Springer C, Bar-Yishay E, Uwayyed K, et al. Corticosteroids do not affect the clinical or physiological status of infants with bronchiolitis. Pediatr Pulmonol. 1990;9(3):181-185.(Randomized, controlled; 14)
-
Dabbous IA, Tkachyk JS, Stamm SJ. A double-blind study on the effects of corticosteroids in the treatment of bronchiolitis. Pediatrics. 1966. 37(3):477-484. (Randomized, controlled; 44)
-
Berger I, Argaman Z, Schwartz SB, et al. Efficacy of corticosteroids in acute bronchiolitis: short-term and long-term follow-up. Pediatr Pulmonol. 1998;26(3):162-166. (Randomized, double-blind, placebo-control; 38)
-
Corneli HM, Zorc JJ, Mahajan P, et al. A multicenter, randomized, controlled trial of dexamethasone for bronchiolitis. N Engl J Med. 2007;357(4):331-339. (Randomized, doubleblind, controlled, multi-center; 600)
-
Mackway-Jones K. Towards evidence based emergency medicine: best BETs from the Manchester Royal Infirmary. Emer Med Journ. 2008;25(1):38. (Systematic review)
-
Plint AC, Johnson DW, Patel H, et al. Epinephrine and dexamethasone in children with bronchiolitis. N Engl J Med. 2009;360(20):2079-2089. (Randomized, double-blind, placebo-control; 800)
-
Kneyber MC, Brandenburg AH, de Groot R, et al. Risk factors for respiratory syncytial virus associated apnoea. Eur J Pediatr. 1998;157(4):331-335. (Retrospective; 185)
-
Purcell K, Fergie J. Driscoll Children’s Hospital respiratory syncytial virus database: risk factors, treatment and hospital course in 3308 infants and young children, 1991 to 2002. Pediatr Infect Dis J. 2004;23(5):418-423. (Prospective, 3308)
-
Willwerth BM, Harper MB, Greenes DS. Identifying hospitalized infants who have bronchiolitis and are at high risk for apnea. Ann Emerg Med. 2006; 48(4):441-447. (Retrospective cohort; 691)
-
Ralston, S. and V. Hill, Incidence of apnea in infants hospitalized with respiratory syncytial virus bronchiolitis: a systematic review. J Pediatr, 2009. 155(5):728-33. (Systematic review)
-
Kho, N. et al. Respiratory syncytial virus infection and neurologic abnormalities: retrospective cohort study. J Child Neurol, 2004. 19(11):859-64. (Retrospective cohort; 236)
-
Sarrell EM, Tal G, Witzling, et al. Nebulized 3% hypertonic saline solution treatment in ambulatory children with viral bronchiolitis decreases symptoms. Chest. 2002;122(6):2015-2020. (Randomized, double-blind, controlled; 65)
-
Grewal S, Ali S, McConnell DW, et al. A randomized trial of nebulized 3% hypertonic saline with epinephrine in the treatment of acute bronchiolitis in the emergency department. Arch Pediatr Adolesc Med. 2009;163(11):1007-1012. (Randomized, double-blind, controlled; 46)
-
Anil AB, Anil M, Saglam AB, et al. High volume normal saline alone is as effective as nebulized salbutamol-normal saline, epinephrine-normal saline, and 3% saline in mild bronchiolitis. Pediatr Pulmonol. 2010;45(1):41-47. (Randomized, double-blind; 186)
-
Kuzik BA, Flavin MP, Kent S, et al. Effect of inhaled hypertonic saline on hospital admission rate in children with viral bronchiolitis: a randomized trial. CJEM. 2010;12(6):477-484. (Randomized, double-blind, controlled; 81)
-
Al-Ansari K, Sakran M, Davidson BL, et al. Nebulized 5% or 3% hypertonic or 0.9% saline for treating acute bronchiolitis in infants. J Pediatr. 2010. 157(4):630-634, 634 e1. (Randomized, double-blind, controlled; 187)
-
U.S. National Institutes of Health. Bronchiolitis and Hypertonic Saline Trials. Available from: http://www.clinicaltrials. gov/ct2/results?term=bronchiolitis+and+hypertonic+saline. (Last visited 6/13/2011).
-
Hollman G, Shen G, Zeng L, et al. Helium-oxygen improves Clinical Asthma Scores in children with acute bronchiolitis. Crit Care Med. 1998. 26(10):1731-1736. (Randomized, doubleblind; 65)
-
Gross MF, Spear RM, Peterson BM. Helium-oxygen mixture does not improve gas exchange in mechanically ventilated children with bronchiolitis. Crit Care. 2000;4(3):188-192. (Controlled, cross-over; 10)
-
Martinon-Torres F, Rodriguez-Nunez A, Martinon-Sanchez JM. Heliox therapy in infants with acute bronchiolitis. Pediatrics. 2002;109(1):68-73. (Controlled; 38)
-
Martinon-Torres F, Rodriguez-Nunez A, Martinon-Sanchez, JM. Nasal continuous positive airway pressure with heliox versus air oxygen in infants with acute bronchiolitis: a crossover study. Pediatrics. 2008. 121(5):e1190-1195. (Prospective,cross-over; 12)
-
Liet JM, Ducrruet T, Gupta V, et al. Heliox inhalation therapy for bronchiolitis in infants. Cochrane Database Syst Rev. 2010;(4):CD006915. (Systematic review)
-
McKiernan C, Chua LC, Vistintainer PF, et al. High flow nasal cannulae therapy in infants with bronchiolitis. J Pediatr. 2010;156(4):634-8. (Retrospective; 115)
-
Javouhey E, Barats A, Richard N, et al. Non-invasive ventilation as primary ventilatory support for infants with severe bronchiolitis. Intensive Care Med. 2008;34(9):1608-1614. (Retrospective;80)
-
Rowe BH, Corticosteroid treatment for acute croup. Ann Emerg Med. 2002;40(3):353-355. (Comment)
-
Donaldson D, Poleski D, Knipple E, et al. Intramuscular versus oral dexamethasone for the treatment of moderateto-severe croup: a randomized, double-blind trial. Acad Emerg Med. 2003;10(1):16-21. (Randomized, double-blind, controlled; 95)
-
Cruz MN, Stewart G, Rosenberg N. Use of dexamethasone in the outpatient management of acute laryngotracheitis. Pediatrics. 1995;96(2 Pt 1):220-223. (Randomized, placebocontrol; 38)
-
Rittichier KK, Ledwith CA. Outpatient treatment of moderate croup with dexamethasone: intramuscular versus oral dosing. Pediatrics. 2000;106(6):1344-1348. (Randomized, single-blind; 277)
-
Bjornson CL, Klassen TP, Williamson J, et al. A randomized trial of a single dose of oral dexamethasone for mild croup. N Engl J Med. 2004;351(13):1306-1313. (Randomized, placebo-controlled, multi-center; 720)
-
Russell K, Wiebe N, Saenz A, et al. Glucocorticoids for croup. (update of Cochrane Database Syst Rev. 2000;(2):CD001955; PMID: 10796674). Cochrane Database of Syst Rev. 2004;(1):CD001955. (Systematic review)
-
Neto GM, Kentab O, Klassen TP, et al. A randomized controlled trial of mist in the acute treatment of moderate croup. Acad Emerg Med. 2002;9(9):873-879. (Randomized, controlled; 71)
-
Moore M, Little P. Humidified air inhalation for treating croup. Cochrane Database of Syst Rev. 2006;(3):CD002870. (Systematic review)
-
Weber JE, Chudnofsky CR, Younger JG, et al. A randomized comparison of helium-oxygen mixture (Heliox) and racemic epinephrine for the treatment of moderate to severe croup. Pediatrics. 2001;107(6):E96. (Randomized; 33)
-
Vorwerk C, Coats T. Towards evidence based emergency medicine: best BETs from the Manchester Royal Infirmary. BET 1: Heliox in croup.(erratum appears in Emerg Med J. 2008;25(9)620). Emerg Med J. 2008;25(6):365-366. (Systematic review)
-
Vorwerk C, Coats T. Heliox for croup in children. Cochrane Database Syst Rev 2010;(2):CD006822. (Systematic review)
-
Daines CL, Wood RE, Boesch RP. Foreign body aspiration: an important etiology of respiratory symptoms in children. J Allergy Clin Immunol. 2008;121(5):1297-1298. (Case report)
-
Cohen S, Avital A. Godfrey S, et al. Suspected foreign body inhalation in children: what are the indications for bronchoscopy? J Pediatr. 2009;155(2):276-280. (Prospective cohort; 142)
-
Portier P, Richet C. De l’action anaphylactique de certains venis. C R Soc Bio. 1902;(54):170-2. (Animal study)
-
The diagnosis and management of anaphylaxis. Joint Task Force on Practice Parameters, American Academy of Allergy, Asthma, and Immunology, American College of Allergy, Asthma and Immunology, and the Joint Council of Allergy, Asthma and Immunology. J Allergy Clin Immunol. 1998;101(6 Pt 2):S465-528. (Guideline)
-
Sampson HA, Muñoz-Furlong A, Bock SA, et al. Symposium on the definition and management of anaphylaxis: summary report. J Allergy Clin Immunol. 2005;115(3):584-591. (Guideline)
-
Barnard JH. Studies of 400 Hymenoptera sting deaths in the United States. J Allergy Clin Immunol. 1973;52(5):259-64. (Case series; 400)
-
Lee JM, Greenes DM. Biphasic anaphylactic reactions in pediatrics. Pediatrics. 2000;106(4)762-766. (retrospective; 108)
-
Sampson HA, Mendelson L, Rosen JP. Fatal and near-fatal anaphylactic reactions to food in children and adolescents. N Engl J Med. 1992;327(6):380-384. (Case-control; 13)
-
Simons FE, Gu X, Johnston LM, et al. Can epinephrine inhalations be substituted for epinephrine injection in children at risk for systemic anaphylaxis? Pediatrics. 2000;106(5):1040-1044. (Randomized, single-blind, placebo-control; 19)
-
Kemp SF, Lockey RF, Simons FE. Epinephrine: the drug of choice for anaphylaxis. A statement of the World Allergy Organization. Allergy. 2008;63(8):1061-1070. (Guideline)
-
The diagnosis and management of anaphylaxis: an updated practice parameter. J Allergy Clin Immunol. 2005;115(3 Suppl 2):S483-523. (Guideline)
-
Pumphrey RS. Fatal posture in anaphylactic shock. J Allergy Clin Immunol. 2003;112(2):451-452. (Letter)
-
Kambam JR, Merrill WH, Smith BE. Histamine-2 receptor blocker in the treatment of protamine related anaphylactoid reactions: two case reports. Can J Anaesth. 1989;36(4):463-5. (Case-report; 2)
-
Alrasbi M, Sheikh A. Comparison of international guidelines for the emergency medical management of anaphylaxis. Allergy. 2007;62(8):838-841. (Meta-analysis)
-
Sampson HA. Anaphylaxis and emergency treatment. Pediatrics. 2003;111(6 Pt 3):1601-1608. (Review)
-
Bock SA, Munoz-Furlong A, Sampson HA. Further fatalities caused by anaphylactic reactions to food, 2001-2006. J Allergy Clin Immunol. 2007. 119(4):1016-1018. (Retrospective)
-
Pumphrey RS, Gowland MH. Further fatal allergic reactions to food in the United Kingdom, 1999-2006. J Allergy Clin Immunol. 2007;119(4):1018-1019. (Retrospective)
-
Salaria M, Singhi SC. Profile of patients attending pediatric emergency service at Chandigarh. Indian J Pediatr. 2003;70(8):621-624. (Retrospective; 9205)
-
Hanvey L, Avard D, Graham I. The Health of Canada’s children: A CICH profile. 2 ed. Canadian issue of Child Health. 1994: Ottawa. (Guideline)
-
Babl FE, Vinci RJ, Bauchner H, et al. Pediatric pre-hospital advanced life support care in an urban setting. Pediatr Emerg Care. 2001;17(1):5-9. (Retrospective; 555)
-
Akinbami LJ, Mooreman JE, Liu X. Asthma prevalence, health care use and mortality: United States, 2005-2009, in National health statistics reports. 2011, National Center for Heath Statisitics: Hyattsville, MD. (Government report)
-
Guidelines for cardiopulmonary resuscitation and emergency cardiac care. Emergency Cardiac Care Committee and Subcommittees, American Heart Association. Part VI. Pediatric advanced life support. JAMA. 1992;268(16):2262-2275. (Guideline)
-
Bardella IJ, Pediatric advanced life support: a review of the AHA recommendations. American Heart Association. Am Fam Physician. 1999;60(6):1743-1750. (Guideline)
-
Allen J. Pulmonary complications of neuromuscular disease: a respiratory mechanics perspective. Paediatr Respir Rev. 2010;11(1):18-23. (Review)
-
Papastamelos C, Panitch HB, England SE, et al. Developmental changes in chest wall compliance in infancy and early childhood. J Appl Physiol. 1995. 78(1):179-184. (Prospective;40)
-
Abu-Shaweesh JM, Martin RJ. Neonatal apnea: what’s new? Pediatr Pulmonol. 2008;43(10):937-944. (Review)
-
Foltin G, Markenson D, Tunik M, et al. Assessment of pediatric patients by emergency medical technicians-basic. Pediatr Emerg Care. 2002;18(2):81-85. (Retrospective; 2430)
-
Gausche M, Lewis Rj, Stratton SJ, et al. Effect of out-ofhospital pediatric endotracheal intubation on survival and neurological outcome: a controlled clinical trial. (erratum appears in JAMA 2000; 283(24):3204). JAMA. 2000;283(6)783- 790. (Prospective, controlled; 830)
-
Wang HE, Yealy DM. Out-of-hospital endotracheal intubation: where are we? Ann Emerg Med. 2006;47(6):532-541. (Review)
-
Sirbaugh PE, Pepe PE, Shook JE, et al. A prospective, population-based study of the demographics, epidemiology, management, and outcome of out-of-hospital pediatric cardiopulmonary arrest. (erratum appears in Ann Emerg Med. 1999 Mar;33(3)358). Ann Emerg Med. 1999;33(2):174-184. (Prospective observational; 300)
-
2005 American Heart Association (AHA) guidelines for cardiopulmonary resuscitation (CPR) and emergency cardiovascular care (ECC) of pediatric and neonatal patients: pediatric basic life support. Pediatrics. 2006;117(5):e989-1004. (Guideline)
-
Workgroup on, E.M.S.M.o.A.E. A model protocol for emergency medical services management of asthma exacerbations. Prehospital Emergency Care. 2006;10(4):418-429. (Guideline)
-
Richmond NJ, Silverman, Kusick M, et al. Out-of-hospital administration of albuterol for asthma by basic life support providers.(erratum appears in Acad Emerg Med. 2005 May;12(6)576). Acad Emerg Med. 2005. 12(5):396-403. (Prospective, observational cohort; 3551)
-
Long SS. Pertussis (Bordetella Pertussis and Bordetella Parapertussis), in Nelson Textbook of Pediatrics, Kliegman, Editor. 2007, Saunders. (Book chapter)
-
Belessis Y, Dixon S, Thomsen A, et al. Risk factors for an intensive care unit admission in children with asthma. Pediatr Pulmonol. 2004;37(3):201-209. (Prospective, case-control; 141)
-
Kotecha S. Chronic Respiratory Complications of Prematurity, in Taussig: Pediatric Respiratory Medicine, 2008 Mosby. (Book chapter)
-
Castro-Rodriguez JA, Holberg CJ, Wright AL, et al. A clinical index to define risk of asthma in young children with recurrent wheezing. Am J Respir Crit Care Med. 2000;162(4 Pt 1):1403-1406. (retrospective; 1246)
-
Lehtinen P, Ruohola, Vanto T, et al. Prednisolone reduces recurrent wheezing after a first wheezing episode associated with rhinovirus infection or eczema. J Allergy Clin Immunol. 2007;119(3):570-575. (Cohort; 118)
-
Panickar J, Lakhanpaul M, Lambert PC, et al. Oral prednisolone for preschool children with acute virus-induced wheezing. N Engl J Med. 2009;360(4):329-338. (Randomized, double-blind, placebo-control; 700)
-
Fleisher GR, Ludwig S. Textbook of pediatric emergency medicine. 6th ed. 2010, Philadelphia: Wolters Kluwer/Lippincott Williams & Wilkins Health. 1970. (Book chapter)
-
Marx JA, Hockberger RS, Walls RM, et al. Rosen’s Emergency Medicine : concepts and clinical practice. 7th ed. 2009, Philadelphia: Mosby/Elsevier. 2 v. (xxxvii, 2604, cviii). (Book chapter)
-
Ralph J, Rivello N, Brown A. Otolaryngologic Procedures, in Robert: Clinical Procedures in Emergency Medicine. 2009, Saunders. (Book Chapter)
-
Mohseni M, Lopez MD. Images in emergency medicine. Uvular angioedema (Quincke’s disease). Ann Emerg Med. 2008;51(1):8, 12. (Case report)
-
WHO, The management of acute respiratory infections in children, in Practical guidelines for outpatient care. 1995, World Health Organization: Geneva. (Guideline)
-
Lynch T, Platt R, Gouin S, et al. Can we predict which children with clinically suspected pneumonia will have the presence of focal infiltrates on chest radiographs? Pediatrics, 2004;113(3 Pt 1):e186-189. (Prospective; 570)
-
Mahabee-Gittens EM, Grupp-Phelan J, Brody AS, et al. Identifying children with pneumonia in the emergency department. Clin Pediatr (Phila). 2005;44(5):427-435. (Prospective cohort; 510)
-
Rothrock SG, Green SM, Fanelli JM, et al. Do published guidelines predict pneumonia in children presenting to an urban ED? Pediatr Emerg Care. 2001;17(4):240-243. (Prospective observational; 329)
-
Shah S, Bachur R, Kim D, et al. Lack of predictive value of tachypnea in the diagnosis of pneumonia in children. Pediatr Infect Dis J. 2010;29(5):406-409. (Prospective; 1622)
-
Neuman MI, Scully KJ, Kim D, et al. Physician assessment of the likelihood of pneumonia in a pediatric emergency department. Pediatr Emerg Care. 2010;26(11):817-822. (Prospective observational; 2071)
-
Kliegman R, Nelson WE. (eds.) Nelson textbook of pediatrics. 18th ed. The Respiratory System, Chapter 370.2. 2007, Saunders: Philadelphia. (Book chapter)
-
Orlow SJ, Isakoff MS, Blei F. Increased risk of symptomatic hemangiomas of the airway in association with cutaneous hemangiomas in a “beard” distribution. J Pediatr. 1997;131(4):643-646. (Case series; 16)
-
Midulla F, Guidi R, Barbato A, et al. Foreign body aspiration in children. Pediatr Int. 2005;47(6):663-8. (Retrospective; 82)
-
Roback MG, Dreitlein DA. Chest radiograph in the evaluation of first time wheezing episodes: review of current clinical practice and efficacy. Pediatr Emerg Care. 1998;14(3):181-184. (Retrospective; 298)
-
Schuh S, Lalani A, Allen U, et al. Evaluation of the utility of radiography in acute bronchiolitis. J Pediatr. 2007;150(4):429-33. (Prospective cohort; 265)
-
Yong JH, Schuh S, Rashidi R, et al. A cost effectiveness analysis of omitting radiography in diagnosis of acute bronchiolitis. Pediatr Pulmonol. 2009;44(2):122-127. (Cost analysis)
-
Farah MM, Padgett LB, McLario DJ, et al. First-time wheezing in infants during respiratory syncytial virus season: chest radiograph findings. Pediatr Emerg Care. 2002;18(5):333-336. (Prospective; 140)
-
Rafei K, Lichenstein R. Airway infectious disease emergencies. Pediatr Clin N America. 2006;53(2):215-242. (Review)
-
Lazor JB, Cunningham MJ, Eavey RD, et al. Comparison of computed tomography and surgical findings in deep neck infections. Otolaryngol Head Neck Surg. 1994;111(6):746-750.(Retrospective; 38)
-
Craig FW, Schunk SE. Retropharyngeal abscess in children: clinical presentation, utility of imaging, and current management. Pediatrics. 2003;111(6 Pt 1):1394-1398. (Retrospective; 64)
-
Al-Sabah B, Bin Saleen H, Hagr A, et al. Retropharyngeal abscess in children: 10-year study. J Otolaryngol. 2004;33(6):352-355. (Retrospective; 68)
-
Page NC, Bauer EM, Lieu JE. Clinical features and treatment of retropharyngeal abscess in children. Otolaryngol Head Neck Surg. 2008;138(3):300-306. (Retrospective cohort; 162)
-
Fleisher GR, Ludwig S. Textbook of pediatric emergency medicine. 6th ed. 2010, Philadelphia: Wolters Kluwer/Lippincott Williams & Wilkins Health. (Book chapter)
-
YildizdaÅŸ D, YapicioÄŸlu H, Yilmaz HL, et al. Correlation of simultaneously obtained capillary, venous, and arterial blood gases of patients in a paediatric intensive care unit. Arch Dis Child. 2004;89(2):176-180. (Prospective; 116)
-
Brandenburg MA, Dire DJ. Comparison of arterial and venous blood gas values in the initial emergency department evaluation of patients with diabetic ketoacidosis. Ann Emerg Med. 1998;31(4):459-65. (Prospective; 44)
-
Malatesha G, Singh NK, Bharija A, et al. Comparison of arterial and venous pH, bicarbonate, PCO2 and PO2 in initial emergency department assessment. Emerg Med J. 2007;24(8):569-571. (Prospective; 95)
-
Koul PA, Khan UH, Wani AA, et al. Comparison and agreement between venous and arterial gas analysis in cardiopulmonary patients in Kashmir valley of the Indian subcontinent. Ann Thorac Med. 2011;6(1):33-37. (Prospective; 100)
-
Abramo TJ, Wiebe RA, Scott SM, et al. Noninvasive capnometry in a pediatric population with respiratory emergencies. Pediatr Emerg Care. 1996;12(4):252-254. (Prospective observational; 85)
-
Corbo J, Bijur, Lahn M, et al. Concordance between capnography and arterial blood gas measurements of carbon dioxide in acute asthma. Ann Emerg Med. 2005;46(4):323-327.(Prospective cohort; 39)
-
Moses JM, Alexander JL, Agus MS. The correlation and level of agreement between end-tidal and blood gas pCO2 in children with respiratory distress: a retrospective analysis. BMC Pediatr. 2009;920. (Retrospective; 80)
-
Egleston CV, Ben Aslam H, Lambert MA. Capnography for monitoring non-intubated spontaneously breathing patients in an emergency room setting. J Acc Emerg Med. 1997;14(4):222-224. (Prospective; 38)
-
Soto RG, Fu ES, Vila H Jr, et al. Capnography accurately detects apnea during monitored anesthesia care. Anesth Analg. 2004;99(2):379-382. (Prospective, blinded; 39)
-
Miner JR, Heegaard W, Plummer D. End-tidal carbon dioxide monitoring during procedural sedation. Acad Emerg Med. 2002;9(4):275-280. (Prospective observational; 74)
-
Burton JH, Harrah JD, Germann CA, et al. Does end-tidal carbon dioxide monitoring detect respiratory events prior to current sedation monitoring practices? Acad Emerg Med. 2006;13(5):500-504. (Prospective; 20)
-
Lightdale JR, Goldmann DA, Feldman HA, et al. Microstream capnography improves patient monitoring during moderate sedation: a randomized, controlled trial. Pediatrics. 2006;117(6):e1170-8. (Randomized, controlled; 174)
-
Practice guidelines for sedation and analgesia by non-anesthesiologists. Anesthesiology. 2002;96(4):1004-1017. (Guideline)
-
Langhan ML, Zonfrillo MR, Spiro DM. Quantitative endtidal carbon dioxide in acute exacerbations of asthma. J Pediatr. 2008;152(6):829-832. (Prospective; 86)
-
Mower WR, Sachs C, Nicklin EL, et al. Pulse oximetry as a fifth pediatric vital sign. Pediatrics. 1997;99(5):681-686. (Prospective, before and after study; 2127)
-
Brown L, Dannenberg B. Pulse oximetry in discharge decision-making: a survey of emergency physicians. CJEM. 2002; 4(6):388-393. (Survey; 182)
-
Brown L, Reiley DG, Jeng A, et al. Bronchiolitis: Can objective criteria predict eligibility for brief hospitalization? CJEM. 2003;5(4):239-244. (Retrospective; 225)
-
Roback MG, Baskin MN. Failure of oxygen saturation and clinical assessment to predict which patients with bronchiolitis discharged from the emergency department will return requiring admission. Pediatr Emerg Care. 1997;13(1):9-11. (Retrospective, case-control; 181)
-
Tanen DA, Trocinski DR. The use of pulse oximetry to exclude pneumonia in children. Am J Emerg Med. 2002;20(6):521-523. (Retrospective, case-control; 803)
-
Curran J, Shah NB, Platt SL. Impact of the Rapid Influenza Test on Evaluation of the Febrile Child in the Emergency Setting. Clin Pediatr Emerg Med. 2008;(9):228-232. (Survey)
-
Melendez E, Harper MB. Utility of sepsis evaluation in infants 90 days of age or younger with fever and clinical bronchiolitis. Pediatr Infect Dis J. 2003; 22(12):1053-1056. (Retrospective; 329)
-
Bilavsky E, Shouval DS, Yarden-Bilavsky H, et al. A prospective study of the risk for serious bacterial infections in hospitalized febrile infants with or without bronchiolitis. Pediatr Infect Dis J. 2008;27(3):269-270.
-
Levine DA, Platt SL, Dayan PS, et al. Risk of serious bacterial infection in young febrile infants with respiratory syncytial virus infections. Pediatrics. 2004;113(6)1728-1734. (Prospective; 312)
-
Titus MO, Wright SW. Prevalence of serious bacterial infections in febrile infants with respiratory syncytial virus infection. Pediatrics. 2003;112(2):282-284. (Retrospective cohort; 174)
-
Bledsoe GH, Schexnayder SM. Pediatric rapid sequence intubation: a review. Pediatr Emerg Care. 2004;20(5):339-344. (Review)
-
Zideman D, Zaritsky A, Carlo W, et al. Airways in pediatric and newborn resuscitation. Ann Emerg Med. 2001;37(4 Suppl):S126-136. (Review)
-
Tait AR, Pandit UA, Voepel-Lewis T, et al. Use of the laryngeal mask airway in children with upper respiratory tract infections: a comparison with endotracheal intubation. Anesth Analg. 1998;86(4):706-711. (Randomized clinical trial; 82)
-
Efrat R, Kadari A, Katz S. The laryngeal mask airway in pediatric anesthesia: experience with 120 patients undergoing elective groin surgery. J Pediatr Surg. 1994;29(2):206-208. (Case series; 120)
-
Parmet JL, Colonna-Romano P, Horrow JC, et al. The laryngeal mask airway reliably provides rescue ventilation in cases of unanticipated difficult tracheal intubation along with difficult mask ventilation. Anesth Analg. 1998;87(3):661-665. (Case series; 17)
-
Guyette FX, Roth KR, LaCovey, et al. Feasibility of laryngeal mask airway use by prehospital personnel in simulated pediatric respiratory arrest. Prehosp Emerg Care. 2007;11(2):245-249. (Prospective intervention study; 13)
-
Barata I. The laryngeal mask airway: prehospital and emergency department use. Emerg Med Clin North Am. 2008;26(4):1069-1083. (Review)
-
Mace SE, Khan N. Needle cricothyrotomy. Emerg Med Clin North Am. 2008;26(4):1085-1101, xi. (Review)
-
Rubio Quiñones F, Muñoz Saez M, Povatos Serrano EM, et al. Magill forceps: a vital forceps. Pediatr Emerg Care. 1995;11(5):302-303. (Case report; 3)
-
Kristjansson S, Berg-Kelly K, Winso E. Inhalation of racemic adrenaline in the treatment of mild and moderately severe croup. Clinical symptom score and oxygen saturation measurements for evaluation of treatment effects. Acta Paediatr. 1994;83(11):1156-1160. (Double-blind, placebo-controlled; 54)
-
Ledwith CA, Shea LM, Mauro RD. Safety and efficacy of nebulized racemic epinephrine in conjunction with oral dexamethasone and mist in the outpatient treatment of croup. Ann Emerg Med. 1995;25(3):331-337. (Observational; 55)
-
Waisman Y, Klein BL, Boenning DA, Young GM, et al. Prospective randomized double-blind study comparing L-epinephrine and racemic epinephrine aerosols in the treatment of laryngotracheitis (croup). Pediatrics. 1992;89(2):302-306. (Randomized, double-blind, controlled; 31)
-
McCracken Jr GH. Etiology and treatment of pneumonia. Pediatr Infec Dis J. 2000;19(4):373-377. (Review)
-
Adirim T. Protecting Children During Disaster: The Federal View. Clin Pediatr Emerg Med. 2009;10(3):164-172. (Comment)
-
Hospitalized patients with novel influenza A (H1N1) virus infection - California, April-May, 2009. MMWR Morb Mortal Wkly Rep, 2009. 58(19):536-541. (Government report)
-
Recommendations for Use of Antiviral Medications for the Management of Influenza in Children and Adolescent for the 2009-2010 Season--Pediatric Supplement for Health Care Providers. (Website) 2009 10/16/09 (cited 2009 10/19/20009); Available from: http://www.cdc.govh1n1flu/recommendations_pediatric_supplement.htm. Last viewed 5/13/2011. (Guideline)
-
Ratjen F, Doring G. Cystic fibrosis. Lancet, 2003;361(9358):681-689. (Review)
-
Vichinsky EP, Neumay LD, Earles AN, et al. Causes and outcomes of the acute chest syndrome in sickle cell disease. National Acute Chest Syndrome Study Group. N Engl J Med. 2000;342(25):1855-1865. (Prospective observational, multicenter; 538)
-
Morris C, Vichinsky E, Styles L. Clinician assessment for acute chest syndrome in febrile patients with sickle cell disease: is it accurate enough? Ann Emerg Med. 1999;34(1):64-69.(Prospective; 73)
-
Wethers DL, Sickle cell disease in childhood: Part II. Diagnosis and treatment of major complications and recent advances in treatment. Am Fam Phys. 2000;62(6):1309-1314. (Review)
-
Vichinsky EP, Haberkern CM, Neumayr, et al. A comparison of conservative and aggressive transfusion regimens in the perioperative management of sickle cell disease. The Preoperative Transfusion in Sickle Cell Disease Study Group. N Engl J Med. 1995;333(4):206-213. (Randomized, multi-center; 604)
-
Vaucher YE. Bronchopulmonary dysplasia: an enduring challenge. Pediatr Rev. 2002;23(10):349-358. (Review)
-
Slonimski M, Aguilera EJ. Atelectasis and mucus plugging in spinal cord injury: case report and therapeutic approaches. J Spinal Cord Med. 2001; 24(4):284-288. (Case Report)
-
Thill PJ, McGuire JK, Baden HP, et al. Noninvasive positivepressure ventilation in children with lower airway obstruction. Pediatr Crit Care Med. 2004;5(4):337-342. (Prospective randomized, cross-over; 20)
-
Carroll CL, Schramm CM. Noninvasive positive pressure ventilation for the treatment of status asthmaticus in children. Ann Allergy Asthma Immunol. 2006;96(3):454-945. (Retrospective; 79)
-
Beers SL, Abramo TJ, Bracken A, et al. Bilevel positive airway pressure in the treatment of status asthmaticus in pediatrics. Am J Emerg Med. 2007; 25(1):6-9. (Retrospective; 83)
-
Thia LP, McKenzie SA, Blyth TP, et al. Randomised controlled trial of nasal continuous positive airways pressure (CPAP) in bronchiolitis. Arch Dis Child. 2008;93(1):45-47. (Randomized, controlled; 31)
-
Morley CJ, Davis PG. Continuous positive airway pressure: scientific and clinical rationale. Curr Opin Pediatr. 2008;20(2):119-124. (Review)
-
Kubicka ZJ, Limauro J, Darnall RA. Heated, humidified high-flow nasal cannula therapy: yet another way to deliver continuous positive airway pressure? Pediatrics. 2008;121(1):82-88. (Prospective; 27)
-
Plant PK, Owen JL, Elliott MW. Early use of non-invasive ventilation for acute exacerbations of chronic obstructive pulmonary disease on general respiratory wards: a multicentre randomised controlled trial. Lancet. 2000;355(9219):1931-1935. (Randomized, controlled, multi-center; 236)
-
Plant PK, Owen JL, Parrott S, et al. Cost effectiveness of ward based non-invasive ventilation for acute exacerbations of chronic obstructive pulmonary disease: economic analysis of randomised controlled trial. BMJ. 2003;326(7396):956. (Cost analysis)
-
Carl JC, Myers TR, Kirchner HL, et al. Comparison of racemic albuterol and levalbuterol for treatment of acute asthma. J Pediatr. 2003;143(6):731-736. (Randomized, blinded; 482)
-
Schreck DM, Babin S. Comparison of racemic albuterol and levalbuterol in the treatment of acute asthma in the ED. Am J Emerg Med. 2005;23(7):842-847. (Retrospective observational; 736)
-
Qureshi F, Zaritsky A, Welch C, et al. Clinical efficacy of racemic albuterol versus levalbuterol for the treatment of acute pediatric asthma. Ann Emerg Med. 2005;46(1):29-36. (Randomized, double-blind, controlled; 129)
-
Hardasmalani MD, DeBari V, Bithoney WG, et al. Levalbuterol versus racemic albuterol in the treatment of acute exacerbation of asthma in children. Pediatr Emerg Care. 2005;21(7):415-419. (Randomized, double-blind; 70)
-
Ralston ME, Euwema MS, Knecht KR, et al. Comparison of levalbuterol and racemic albuterol combined with ipratropium bromide in acute pediatric asthma: a randomized controlled trial. J Emerg Med. 2005;29(1):29-35. (Randomized,double-blind, controlled; 833)
-
Andrews T, McGintee E, Mittal MK, et al. High-dose continuous nebulized levalbuterol for pediatric status asthmaticus: a randomized trial. J Pediatr. 2009;155(2):205-210 (Randomized, double-blind; 81)
-
Green SM, Krauss B. Ketamine is a safe, effective, and appropriate technique for emergency department paediatric procedural sedation. Emerg Med J. 2004;21(3):271-272. (Review)
-
Eid N, Yandell B, Howell L, et al. Can peak expiratory flow predict airflow obstruction in children with asthma? Pediatrics. 2000;105(2):354-358. (Retrospective; 244)