Table of Contents
-
Abstract
-
Case Presentations
-
Introduction
-
Critical Appraisal Of The Literature
-
Relevant Practice Guidelines
-
Classification Of Headaches
-
Tension-Type Headaches
-
Migraine Headaches
-
Cluster Headaches
-
Other Primary Headaches
-
Pathophysiology
-
Differential Diagnosis
-
Prehospital Care
-
Emergency Department Evaluation
-
History
-
Physical Examination
-
Neurologic Examination
-
Ophthalmologic Examination
-
Head And Neck Examination
-
Other Examinations
-
Diagnostic Studies
-
Making The Diagnosis
-
Treatment
-
NSAIDs
-
Ibuprofen
-
Aspirin
-
Naproxen
-
Diclofenac
-
Ketorolac
-
Acetaminophen
-
Ergot
-
Neuroleptics
-
Chlorpromazine (Thorazine®)
-
Metoclopramide (Maxolon®, Metozolv®, Reglan®)
-
Prochlorperazine (Compazine®, Compro®)
-
Butyrophenones
-
Neuroleptics Summary
-
Triptans
-
Opioids
-
Steroids
-
Treatment For Cluster Headache
-
Treatment Summary
-
Special Circumstances
-
Pediatric Patients
-
Pregnant And Postpartum Patients
-
Controversies And Cutting Edge
-
Disposition
-
Summary
-
Risk Management Pitfalls For Primary Headache
-
Cost-Effective Strategies For Primary Headache
-
Case Conclusions
-
Clinical Pathway For Treatment Of Primary Headache
-
Tables and Figures
-
Table 1. ICHD-2 Primary Headace Diagnostic Criteria
-
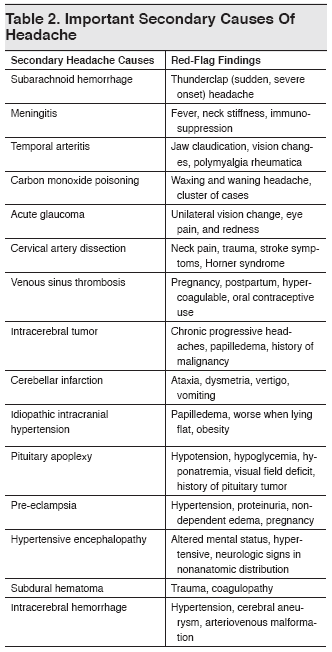
Table 2. Important Secondary Causes Of Headache
-
Table 3. Cincinnati Prehospital Stroke Scale
-
Table 4. Red-Flag Signs And Symptoms Of Dangerous Secondary Headaches
-
Table 5. General History Questions For Evaluation Of Headache
-
Table 6. Selected Concerning Neurologic Examination Findings For The Headache Patient
-
Table 7. Example Physical Examination For Emergency Patient With Headache
-
Table 8. Excluding Secondary Causes Of Headache, By Study
-
Table 9. Medications For Primary Headache, Dosing, And American Academy Of Neurology Quality Of Evidence
-
Table 10. Cochrane Review Summary Of Percentage Of Patients With Pain Relief Or Pain-Free Using Various Formulations Of Sumatriptan
-
Table 11. Contraindications For Triptan Use
-
Table 12. Patterns Of Childhood Headaches
-
Table 13. Medications For Childhood Headaches
-
Table 14. Medications For Headache In Pregnancy, With FDA Safety Guidelines
-
Table 15. CMS OP-15 Exclusion Criteria
-
Table 16. Sample Discharge Instructions
-
References
Abstract
Approximately 2.1 million patients per year present to United States emergency departments with a primary headache disorder. For emergency clinicians, the responsibility is twofold: First, exclude causes of headaches that pose immediate threats to the life and welfare of patients. Second, provide safe, effective, and rapid treatment of symptoms, while facilitating discharge from the emergency department with appropriate follow-up. While emergency management focuses on identification and treatment of life-threatening causes of headache, such as subarachnoid hemorrhage or bacterial meningitis, there is a tendency to misdiagnose specific primary headache disorders and fail to provide consistent, effective treatments in accordance with published guidelines. These mistakes can be avoided by resisting the temptation to label patients with specific primary headache diagnoses and by adopting a consistent, reproducible strategy for treatment of primary headache disorders in the emergency department that is evidence-based and effective.
Case Presentations
You arrive for your shift in the ED and are greeted by a trio of patients with a chief concern of headache. The first is a 10-year-old boy brought by his parents for the evaluation of moderate-intensity frontal headaches that have been going on for several months. The headaches occur in the morning, resolve by the afternoon, and are not changing in character or frequency. He has no other symptoms and appears very well on your exam. The parents are concerned that their child has a brain tumor and are requesting a head CT.
The second patient is a 46-year-old female with a history of migraine headaches who presents with a severe, constant pain that started suddenly while running. She admits this “feels different than my normal headaches.” On examination, she appears ill and is vomiting. Her neurologic examination demonstrates mild neck stiffness. She asks for a refill of her sumatriptan, which “always works for my headaches.”
The third patient arrives by ambulance. She is a 27-year-old “frequent flyer.” She describes her typical migraine headache, not controlled with home medications. Her vital signs and examination are unremarkable. You would like to treat her quickly and effectively, knowing that, if you do not, she will make the rest of your day difficult
Feeling your own head starting to pound, you take a deep breath, grab the charts, and start your day, hoping that you don’t become the fourth patient with a headache.
Introduction
The prevalence of headaches is staggering. It is estimated that almost one-half of the world’s adult population suffers from a headache disorder. While the vast majority of headache patients do not visit the emergency department (ED) for care, headache remains the fifth most common chief complaint, comprising approximately 2% of all ED visits in the United States.1-5 Given an average cost of $1800 per patient visit, this translates to billions of dollars per year in healthcare costs.6 While emergency management focuses on identification and treatment of life-threatening causes of headache, such as subarachnoid hemorrhage (SAH) or bacterial meningitis, there is a tendency to misdiagnose specific primary headache disorders and fail to provide consistent, effective treatments in accordance with published guidelines.7,8
Headaches are commonly classified into 2 groups: (1) primary headache disorders, where the etiology is unknown, and (2) secondary headache disorders, where the headache is attributed to a specific underlying cause.9 (See Table 1.) While emergency medicine training focuses on the identification and management of dangerous secondary causes of headache, the vast majority of patients who present to the ED suffer from a primary headache disorder. As such, it is helpful to use evidence-based strategies to diagnose, manage, and treat these patients. This issue of Emergency Medicine Practice discusses the initial workup and management of patients with primary headache disorders, with special detail to classification and medication options. Common pitfalls associated with the care of the headache patient are also discussed. Finally, basic algorithms will be presented to aid the emergency clinician in the treatment and disposition of the next headache patient.
For more information on diagnosis and treatment of headache in the ED, see the September 2010 issue of EM Practice Guidelines Update, “Current Guidelines For Management Of Headache In the Emergency Department,” and the February 2010 issue of Pediatric Emergency Medicine Practice, “Pediatric Migraine Headache: An Evidence-Based Approach.”
Critical Appraisal Of The Literature
The available literature on headache disorders is sizeable. A literature search was performed using PubMed online with the following search terms: emergency headache, emergency migraine, emergency tension headache, and migraine treatment. Approximately 2400 articles from 1960 to present were reviewed. The National Guideline Clearinghouse (www.guideline.gov) and the Cochrane Database of Systematic Reviews were searched with the term headache and included 7 and 15 review articles, respectively. Guidelines released by the American College of Emergency Physicians (ACEP) and the American Academy of Neurology (AAN) were also searched. The Canadian, French, and European neurology guidelines were also reviewed. To find additional primary literature, a search for headache and migraine was performed in the following emergency medicine journals: Annals of Emergency Medicine, the American Journal of Emergency Medicine, Academic Emergency Medicine, BMC Emergency Medicine, Canadian Journal of Emergency Medicine, Emergency Medicine Clinics of North America, European Journal of Emergency Medicine, Journal of Emergency Medicine, and Western Journal of Emergency Medicine. The bibliographies from these articles were examined to verify accurate representation from the literature.
Risk Management Pitfalls For Primary Headache
-
“She has a history of migraines; I assumed this headache was a migraine as well.”
Emergency clinicians must be careful not to anchor on prior headache diagnoses. The primary goal is to rule out dangerous causes of headaches, even in those who have a history of benign headaches. Patients with migraines or tension headaches can still suffer from meningitis, SAH, or other causes of serious or secondary headaches.
-
“I gave him migraine-specific medicine, and his headache got better. I thought that meant his headache had to be a migraine.”
Given the common pain pathway of headaches, a patient’s response to medication should not be used to aid in diagnosis of the headache disorder. Many case reports and case series have demonstrated that SAH and pain from structural brain lesions respond to triptans, neuroleptics, and ergots.27-30
-
“I thought the patient had a new tension-type headache. I forgot to ask about HIV status.”
While some red flags—such as fever and focal neurological deficits—are apparent on examination, it is the emergency clinician’s job to evaluate all red-flag signs and symptoms. Specifically, history of HIV or cancer should lower the threshold for diagnostic imaging, given that secondary headaches can present with apparently benign symptoms.
-
“I try to provide a specific diagnosis for every primary headache patient according to ICHD-2 guidelines.”
Studies have demonstrated that it is difficult to assign a specific headache diagnosis in the emergency setting. Primary headache disorders have variable presentations and often require multiple similar headaches for diagnosis by ICHD-2 guidelines. Further, an incorrect diagnosis can mislabel a patient with a chronic headache disorder, leading to anchoring bias by future physicians.151
-
“I only use opioids to treat primary headaches.”
Repeated opioid use may precipitate chronic migraines and the phenomenon of the “frequent flyer” patient, who becomes dependent on increasing doses of opioids for headache treatment. With many other appropriate drug choices, we do not recommend opioids as monotherapy.152 If opioids are needed, we recommend them in combination with other medications and only in the acute setting.
-
“I never refer my primary headache patients for specific outpatient follow-up.”
Specialist consultants, whether inhospital or outpatient, can develop specific plans for the prevention of primary headaches as well as home treatment strategies to avoid ED visits. Primary headache patients with multiple visits to the ED should have specific and appropriate outpatient follow-up.
-
“I try to make the patient pain-free prior to discharge.”
It is difficult to alleviate all pain in many patients suffering from primary headache disorders.153 We recommend talking with patients and setting appropriate expectations for controlling and managing pain, and working to provide appropriate follow-up and specific return precautions.
-
“I forgot to tell the patient the side effect of the medication I gave.”
Many primary headache medications, although benign, can have uncomfortable side effects, including chest tightness and tingling for triptans and akathisia for neuroleptics. It is important to inform patients of these common side effects before giving medications. If not, the experience of the side effect may only serve to worsen their primary headache.
-
“I screen with neuroimaging all first-time patients that I believe have a primary headache disorder.”
Neuroimaging is not indicated for patients with primary headache disorders. It is costly, is time-consuming, and carries risks of radiation. Once dangerous secondary causes of headache are excluded by history and physical examination, laboratory tests and neuroimaging are not indicated.34
-
“If my patient bounces back to the ED with recurrent pain, then I have done something wrong.”
Patients with primary headaches often have recurrence of their pain. In fact, studies have been unable to discover factors that reliably predict which ED headache patients will have recurrence of pain. This should not be seen as a medical error, but rather, a natural progression of the disease. It does, however, emphasize the importance of appropriate discharge instructions to prepare patients if their headache returns.149
Tables and Figures
References
Evidence-based medicine requires a critical appraisal of the literature based upon study methodology and number of subjects. Not all references are equally robust. The findings of a large, prospective, randomized, and blinded trial should carry more weight than a case report.
To help the reader judge the strength of each reference, pertinent information about the study will be included in bold type following the reference, where available. In addition, the most informative references cited in this paper, as determined by the authors, are noted by an asterisk (*) next to the number of the reference.
-
Stovner LJ, Hagen K, Jensen R, et al. The global burden of headache: a documentation of headache prevalence and disability worldwide. Cephalalgia. 2007;27(3):193-210. (Systematic review)
-
Friedman BW, Serrano D, Reed M, et al. Use of the emergency department for severe headache. A population-based study. Headache. 2009;49(1):21-30. (Survey; 18,000 participants)
-
McCaig LF, Burt CW. National hospital ambulatory medical care survey: 2003 emergency department summary. Adv Data. 2005;348:1-38. (Survey)
-
Vinson DR. Treatment patterns of isolated benign headache in US emergency departments. Ann Emerg Med. 2002;39(3):215-222. (Survey)
-
Goldstein JN, Camargo CA Jr, Pelletier AJ et al. Headache in United States emergency departments: demographics, work-up and frequency of pathological diagnoses. Cephalagia. 2006;26(6):684-690. (Survey review)
-
Hawkins K, Wang S, Rupnow M. Direct cost burden among insured US employees with migraine. Headache. 2008;48(4):553-563. (Survey)
-
* Friedman BW, et al. Applying the international classification of headache disorders to the emergency department: an assessment of reproducibility and the frequency with which a unique diagnosis can be assigned to every acute headache presentation. Ann Emerg Med. 2007;49(4):409-419. (Prospective interview, chart review; 480 patients)
-
Gupta MX, Silberstein SD, Young WB, et al. Less is not more: underutilization of headache medication in a university hospital emergency department. Headache. 2007;47(8):1125-1133. (Prospective survey; 219 patients)
-
Headache Classification Subcommittee of the International Headache Society. The international classification of headache disorders, 2nd edition. Cephalalgia. 2004;24 Suppl 1:9-160. (Guidelines)
-
* American College of Emergency Physicians. Clinical policy for the initial approach to adolescents and adults presenting to the emergency department with a chief complaint of headache. Ann Emerg Med. 1996;27(6):821-844. (Guidelines)
-
American College of Emergency Physicians. Clinical policy: critical issues in the evaluation and management of adult patients presenting to the emergency department with acute headache. Ann Emerg Med. January 2002;39(1):108-122. (Guidelines)
-
Edlow JA, Panagos PD, Godwin SA, et al. Clinical policy: critical issues in the evaluation and management of adult patients presenting to the emergency department with acute headache. Ann Emerg Med. 2008;52(4):407-436. (Guidelines)
-
* Silberstein SD. Practice parameter: evidence-based guidelines for migraine headache (an evidence-based review): report of the Quality Standards Subcommittee of the American Academy of Neurology. Neurology. 2000;55(6):754-762. (Guideline)
-
Pryse-Phillips WE, Dodick DW, Edmeads JG, et al. Guidelines for the diagnosis and management of migraine in clinical practice. CMAJ. 1997;156(9):1273-1287. (Guidelines)
-
Ducharme J. Canadian Association of Emergency Physicians guidelines for the acute management of migraine headache. J Emerg Med. 1999;17(1):137-144. (Review article)
-
Evers S, Afra A, Frese P, et al. EFNS guideline on the drug treatment of migraine – revised report of an EFNS task force. Eur J Neurol. 2009;16(9):968-981. (Guideline)
-
Géraud G, Lantéri-Minet M, Lucas C, et al. French guidelines for the diagnosis and management of migraine in adult and children. Clin Ther. 2004;26(8):1305-1318. (Guideline)
-
Olesen J. The international classification of headache disorders. Headache. 2008;48(5): 691-693. (Commentary)
-
Schwartz BS, Stewart WF, Simon D, et al. Epidemiology of tension-type headache. JAMA. 1998;279(5):381-383. (Telephone survey; 13,000 participants)
-
Stewart WF, Lipton RB, Celentano DD, et al. Prevalence of migraine headache in the United States. Relation to age,income, race, and other sociodemographic factors. JAMA. 1992;267(1):64–69. (Survey; 20,000 patients)
-
Lipton RB, Stewart WF, Diamond S, et al. Prevalence and burden of migraine in the United States: data from the American Migraine Study II. Headache. 2001;41(7):646–657. (Survey; 30,000 patients)
-
Lipton RB, Bigal ME, Diamond M, et al. Migraine prevalence, disease burden, and the need for preventive therapy. Neurology. 2007;68(5):343–349. (Survey; 160,000 participants)
-
Robbins MS, Lipton RB. The epidemiology of primary headache disorders. Semin Neurol. 2010;30(2):107-119. (Review article)
-
Edvinsson L, Uddman R. Neurobiology in primary headaches. Brain Res Brain Res Rev. 2005;48(3):438-456. (Review paper)
-
Edvinsson L. Tracing neural connections to pain pathways with relevance to primary headaches. Cephalalgia. 2011;31(6):737-747. (Review paper)
-
Goadsby PJ. Pathophysiology of migraine. Neurol Clin. 2009;27(2):335-360. (Review paper)
-
Pope JV, Edlow JA. Favorable Response to Analgesics does not predict a benign etiology of headache. Headache. 2008; 48:944-950. (literature review)
-
Rosenberg JH,Silberstein SD. The Headache of SAH responds to Sumatriptan. Headache. 2005; 45: 597-598. (Case report)
-
Seymour JJ, Moscati RM, Jehle DV. Response of headaches to nonnarcotic analgesics resulting in missed intracranial hemorrhage. American Journal of Emergency Medicine. 1995; 13:43-45. (case series 3 patients)
-
Forsyth PA, Posner JB. Headaches in patients with brain tumors: a study of 111 patients. Neurology 1993; 43: 1678-1683. (observational)
-
Kothari RU, Pancioli A, Liu T et al. Cincinnati prehospital stroke scale. Reproducibility and validity. Ann Emerg Med. 1999;33:373-378. (Prospective survey; 860 patients)
-
Perry JJ, Stiell IG, Sivilotti ML, et al. High-risk clinical characteristics for subarachnoid haemorrhage in patients with acute headache: prospective cohort study. BMJ. 2010;341:c5204. doi:10.1136/bmj.c5204 (Prospective cohort; 1999 patients)
-
Mayer PL, Awad lA, Todor R, et al. Misdiagnosis of symptomatic cerebral aneurysm. Prevalence and correlation with outcome at our institutions. Stroke. 1996;27(9):1558-1563.
-
* Detsky ME, McDonald DR, Baerlocher MO. Does this patient with headache have a migraine or need neuroimaging? JAMA. 2006;296(10):1274-1283. (Systematic review)
-
Waghdhare S, Kalantri A, Joshi R, et al. Accuracy of physical signs for detecting meningitis: A hospital-based diagnostic accuracy study. Clin Neurol Neurosurg. 2010;112(9)752-757. (Double-blind cross-sectional study; 190 patients)
-
Kaniecki R. Headache assessment and management. JAMA. 2003;289(11):1430-1433. (Review article)
-
Lipton RB, Cady RK, Stewart WF, et al. Diagnostic lessons from the Spectrum Study. Neurology. 2002;58(9 Suppl 6):S27-S31. (Review)
-
Michel P, Henry P, Letenneur L, et al. Diagnostic screen for assessment of the IHS criteria for migraine by general practitioners. Cephalalgia. 1993;13(Suppl 12):54-59. (Survey; 1049 participants)
-
Vinson DR, Hurtado T, Vandenberg JT, et al. Variations among emergency departments in the treatment of benign headaches. Ann Emerg Med. 2003;41(1):90-97. (Retrospective survey)
-
Miner JR, Smith SW, Moore J, et al. Sumatriptan for the treatment of undifferentiated primary headaches in the ED. Am J Emerg Med. 2007;25(1):60-64. (Prospective observational; 147 patients)
-
Trainor A, Miner J. Pain treatment and relief among patients with primary headache subtypes in the ED. Am J Emerg Med. 2008;26:1029. (Prospective observational; 180 patients)
-
Kelley NE, Tepper DE. Rescue therapy for acute migraine, part 3: opioids, NSAIDs, steroids, and post-discharge medications. Headache. 2012;52(3):467-482. (Review)
-
Rabbie R, Derry S, Moore RA, et al. Ibuprofen with or without an antiemetic for acute migraine headaches in adults. Cochrane Database Syst Rev. 2010; 10:CD008039. (Review)
-
Codispoti JR, Prior MJ, Fu M, et al. Efficacy of nonprescription doses of ibuprofen for treating migraine headache. A randomized controlled trial. Headache. 2001;41(7): 665-679. (Placebo-controlled randomized controlled trial; 660 patients, outpatient setting)
-
Diener HC, Bussone G, de Liano H, et al. Placebo-controlled comparison of effervescent acetylsalicylic acid, sumatriptan and ibuprofen in the treatment of migraine attacks. Cephalalgia. 2004;24:947–954. (Randomized controlled trial; 312 patients, outpatient setting)
-
Kirthi V, Derry S, Moore RA, et al. Aspirin with or without an antiemetic for acute migraine headaches in adults. Cochrane Database Syst Rev. 2010;4:CD008041. (Meta-analysis)
-
Suthisisang CC, Poolsup N, Suksomboon N, et al. Meta-analysis of the efficacy and safety of naproxen sodium in the acute treatment of migraines. Headache. 2010;50(5):808-818. (Meta-analysis)
-
Derry S, Rabbie R, Moore RA. Diclofenac with or without an antiemetic for acute migraine headaches in adults. Cochrane Database Syst Rev. 2012;2:CD008783. (Review)
-
Turturro MA, Paris PM, Seaberg DC. Intramuscular ketorolac versus oral ibuprofen in acute musculoskeletal pain. Ann Emerg Med. 1995;26:1(2)17-120. (Randomized controlled trial; 82 patients)
-
Neighbor ML, Puntillo KA. Intramuscular ketorolac vs oral ibuprofen in emergency department patients with acute pain. Acad Emerg Med. 1998;5(2):118-122. (Randomized controlled trial; 119 patients)
-
Shrestha M, Singh R, Moreden J et al. Ketorolac vs chlorpromazine in the treatment of acute migraine without aura. A prospective, randomized, double-blind trial. Arch Intern Med. 1996;156(15):1725-1728. (Randomized controlled trial; 30 patients)
-
Duarte C, Dunaway F, Turner L, et al. Ketorolac versus meperidine and hydroxyzine in the treatment of acute migraine headache: a randomized, prospective, double-blind trial. Ann Emerg Med. 1992;21(9):1116-1121. (Randomized controlled trial; 47 patients)
-
Larkin GL, Prescott JE. A randomized, double-blind, comparative study of the efficacy of ketorolac tromethamine versus meperidine in the treatment of severe migraine. Ann Emerg Med. 1992;21(8):919-924. (Randomized controlled trial; 31 patients)
-
Davis CP, Torre PR, Williams C, et al. Ketorolac versus meperidine-plus-promethazine treatment of migraine headache: evaluations by patients. Am J Emerg Med. 1995;13(2):146-150. (Randomized controlled trial; 42 patients)
-
Meredith JT, Wait S, Brewer KL. A prospective double-blind study of nasal sumatriptan versus IV ketorolac in migraine. Am J Emerg Med. 2003;21(3):173-175. (Randomized controlled trial; 29 patients)
-
Seim MB, March JA, Dunn KA. Intravenous ketorolac vs intravenous prochlorperazine for the treatment of migraine headaches. Acad Emerg Med. 1998;5(6):573-576. (Randomized controlled trial; 64 patients)
-
Jakubowski M, Levy D, Goor-Aryeh I, et al. Terminating migraine with allodynia and ongoing central sensitization using parenteral administration of COX1/COX2 inhibitors. Headache. 2005;45(7):850-861.
-
Derry S, Moore RA, McQuay HJ. Paracetamol (acetaminophen) with or without an antiemetic for acute migraine headaches in adults. Cochrane Database Syst Rev. 2010;11:CD008040. (Review)
-
McBride JT. The association of acetaminophen and asthma prevalence and severity. Pediatrics. 2011;128(6):1181-1185. (Review)
-
Goldstein J, Silberstein SD, Saper JR, et al. Acetaminophen, aspirin, and caffeine in combination versus ibuprofen for acute migraine: results from a multicenter, double-blind, randomized, parallel-group, single-dose, placebo-controlled study. Headache. 2006;46(3):444-453. (Randomized controlled trial; 1555 patients)
-
Coleman I, Brown MD, Innes GD, et al. Parenteral dihydroergotamine for acute migraine headache: a systematic review of the literature. Ann Emerg Med. 2005;45(4):393-401. (Systematic review)
-
Kelley NE, Tepper DE. Rescue therapy for acute migraine, part 2: neuroleptics, antihistamines, and others. Headache. 2012;52(2):292-306. (Review)
-
McEwen JI, O’Connor HM, Dinsdale HB. Treatment of migraine with intramuscular chlorpromazine. Ann Emerg Med. 1987;16(7):758-763. (Randomized controlled trial; 36 patients)
-
Bigal ME, Bordini CA, Speciali JG. Intravenous chlorpromazine in the emergency department treatment of migraine: A randomized controlled trial. J Emerg Med. 2002;23(2):141-148. (Randomized controlled trial; 60 patients)
-
Lane PL, McLellan BA, Baggoley CJ. Comparative efficacy of chlorpromazine and meperidine with dimenhydrinate in migraine headache. Ann Emerg Med. 1989;18(4):360-365. (Randomized controlled trial; 46 patients)
-
Bell R, Montoya D, Shuaib A, et al. A comparative trial of three agents in the treatment of acute migraine headache. Ann Emerg Med 1990;19(10):1079-1082. (Randomized controlled trial; 76 patients)
-
Kelly AM, Ardagh M, Curry C, et al. Intravenous chlorpromazine vs intramuscular sumatriptan for acute migraine. Ann Emerg Med. 1997;14(4):209-211. (Randomized controlled trial; 43 patients)
-
Tek DS, McClellan DS, Olshaker JS, et al. A prospective, double-blind study of metoclopramide hydrochloride for the control of migraine in the emergency department. Ann Emerg Med. 1990;19(10):1083-1087. (Randomized controlled trial; 67 patients)
-
Cete Y, Doara B, Ertan C, et al. A randomized prospective placebo-controlled study of intravenous magnesium sulphate vs metoclopramide in the management of acute migraine attacks in the emergency department. Cephalagia. 2005;25(3):199-204. (Randomized controlled trial; 114 patients)
-
Tfelt-Hansen P, Olesen J, Aebelholt-Krabbe A, et al. A double-blind study of metoclopramide in the treatment of migraine attacks. J Neurol Neurosurg Psychiatry. 1980;43(4):369-371. (Randomized controlled trial; 150 patients)
-
Colman I, Brown M, Innes GD, et al. Parenteral metoclopramide for acute migraine: meta-analysis of randomised controlled trials. BMJ. 2004;329(7479):1369-1373. (Meta-analysis)
-
Friedman BW, Corbo J, Lipton RB, et al. A trial of metoclopramide vs sumatriptan for the emergency department treatment of migraines. Neurology. 2005;64(3):463-468. (Randomized controlled trial; 202 patients)
-
Ellis GL, Delaney J, DeHart DA, et al. The efficacy of metoclopramide in the treatment of migraine headache. Ann Emerg Med. 1993;22(2):191-195. (Randomized controlled trial; 40 patients)
-
Jones J, Sklar D, Dougherty J, et al. Randomized double-blind trial of intravenous prochlorperazine for the treatment of acute headache. JAMA. 1989;261(8):1174-1176. (Randomized controlled trial; 82 patients)
-
Coppola M, Yealy DM, Leibold RA. Randomized, placebo-controlled evaluation of prochlorperazine versus metoclopramide for emergency department treatment of migraine headaches. Ann Emerg Med. 1995;26(5):541-546. (Randomized controlled trial; 70 patients)
-
Friedman BW, Esses D, Solorzano C, et al. A randomized controlled trial of prochlorperazine versus metoclopramide for treatment of acute migraine. Ann Emerg Med. 2008;52(4):399-406. (Randomized controlled trial; 77 patients)
-
Jones J, Pack S, Chun E. Intramuscular prochlorperazine versus metoclopramide as single agent therapy for the treatment of acute migraine headache. Am J Emerg Med. 1996;14(3):262-265. (Randomized controlled trial; 86 patients)
-
Kostic MA, Gutierrez FJ, Rieg TS, et al. A prospective randomized trial of intravenous prochlorperazine versus subcutaneous sumatriptan in acute migraine therapy in the emergency department. Ann Emerg Med. 2010;56(1):1-6. (Randomized controlled trial; 68 patients)
-
Tanen DA, Miller S, French T. Intravenous sodium valproate versus prochlorperazine for the emergency department treatment of acute migraine headaches: a prospective, randomized, double blind trial. Ann Emerg Med. 2003; 41(6): 847-853. (Randomized controlled trial; 40 patients)
-
Miller MA, Levsky ME, Enslow W, et al. Randomized evaluation of octreotide vs prochlorperazine for ED treatment of migraine headache. Am J Emerg Med. 2009;27(2):160-164. (Randomized controlled trial; 44 patients)
-
Callan JE, Kostic MA, Bachrach EA et al. Prochlorperazine vs promethazine for headache treatment in the emergency department: A randomized controlled trial. J Emerg Med. 2008;35(3):247-253. (Randomized controlled trial; 70 patients)
-
Drotts DL, Vinson DR. Prochlorperazine induces akathisia in emergency patients. Ann Emerg Med. 1999;34(4 Pt 1):469-475. (Prospective observational 140 patients)
-
Regan LA, Hoffman RS, Nelson LS. Slower infusion of metoclopramide decreases the rate of akathisia. Am J Emerg Med. 2009;27(4):475-480. (Randomized controlled trial; 127 patients)
-
Vinson DR, Migala AF, Quesenberry CP. Slow infusion for the prevention of akathisia induced by prochlorperazine: A randomized controlled trial. J Emerg Med. 2001;20(2):113-119. (Randomized controlled trial; 160 patients)
-
Vinson DR, Drotts DL. Diphenhydramine for the prevention of akathisia induced by prochlorperazine: a randomized, controlled trial. Ann Emerg Med. 2001;37(2):125-131. (Randomized controlled trial; 100 patients)
-
Friedman BW, Bender B, Davitt M, et al. A randomized trial of diphenhydramine as prophylaxis against metoclopramide induced akathisia in nauseated emergency department patients. Ann Emerg Med. 2009;53(3):379-385. (Randomized controlled trial; 289 patients)
-
Honkaniemi J, Liimatainen S, Rainesalo S, et al. Haloperidol in the acute treatment of migraine: A randomized, double-blind, placebo-controlled study. Headache. 2006;46(5):781-787. (Randomized double-blinded, placebo-controlled trial; 40 patients)
-
Silberstein SD, Young WB, Mendizabal JE, et al. Acute migraine treatment with droperidol: A randomized, double-blind, placebo-controlled trial. Neurology. 2003;60(2):315-321. (Randomized double-blinded, placebo-controlled trial; 331 patients)
-
Richman PB, Allegra J, Eskin B, et al. A randomized clinical trial to assess the efficacy of intramuscular droperidol for the treatment of acute migraine headache. Am J Emerg Med. 2002;20(1):39-42. (Randomized, double-blinded; 29 patients)
-
Miner JR, Fish SJ, Smith SW, et al. Droperidol vs prochlorperazine for benign headaches in the emergency department. Acad Emerg Med. 2001;8(9):873-879. (Prospective single-blinded randomized controlled trial; 162 patients)
-
Weaver CS, Jones JB, Chisholm CD, et al. Droperidol vs prochlorperazine for the treatment of acute headache. J Emerg Med. 2004;26(2):145-150. (Randomized, blinded; 96 patients)
-
Kelley NE, Tepper DE. Rescue therapy for acute migraine, part 1: triptans, dihydroergotamine, and magnesium. Headache. 2012;52(1):114-128. (Review)
-
Tfelt-Hansen P, De Vries P, Saxena PR. Triptans in migraine: a comparative review of pharmacology, pharmacokinetics and efficacy. Drugs. 2000;60(6):1259-1287. (Review)
-
Derry CJ, Derry S, Moore RA. Sumatriptan (rectal route of administration) for acute migraine attacks in adults. Cochrane Database Syst Rev. 2012;2:CD009664. DOI: 10.1002/14651858.CD009664. (Meta-analysis)
-
Derry CJ, Derry S, Moore RA. Sumatriptan (subcutaneous route of administration) for acute migraine attacks in adults. Cochrane Database Syst Rev. 2012;2:CD009665. DOI: 10.1002/14651858.CD009665. (Meta-analysis)
-
Derry CJ, Derry S, Moore RA. Sumatriptan (intranasal route of administration) for acute migraine attacks in adults. Cochrane Database Syst Rev. 2012;2: CD009663. DOI: 10.1002/14651858.CD009663. (Meta-analysis)
-
Derry CJ, Derry S, Moore RA. Sumatriptan (oral route of administration) for acute migraine attacks in adults. Cochrane Database Syst Rev. 2012;2: CD008615. DOI: 10.1002/14651858.CD008615.pub2. (Meta-analysis)
-
Visser WH, de Vriend RH, Jaspers MW, et al. Sumatriptan in clinical practice: a 2-year review of 453 migraine patients. Neurology.1996;47(1):46-51. (Retrospective survey; 735 patients)
-
Ferrari MD, James MH, Bates D, et al. Oral sumatriptan: effect of a second dose, and treatment of headache recurrence. Cephalalgia. 1994;14(5):330-338. (Randomized controlled trial; 1291 patients)
-
Scott RJ, Aitchison WR, Barker PR, et al. Oral sumatriptan in the acute treatment of migraine and migraine recurrence in general practice. QJM. 1996;89(8):613-622. (Randomized controlled trial; 1440 patients)
-
Rapoport A, Visser WH, Cutler NR, et al. Oral sumatriptan in preventing headache recurrence after treatment of migraine attacks with subcutaneous sumatriptan. Neurology. 1995;45(8):1505-1509. (Randomized controlled trial; 667 patients)
-
Welch KM, Mathew NT, Stone P, et al. Tolerability of sumatriptan: clinical trials and post-marketing experience. Cephalalgia. 2000;20(8):687-695. (Retrospective review)
-
Evans RW, Tepper SJ, Shapiro RE, et al. The FDA alert on serotonin syndrome with use of triptans combined with selective serotonin reuptake inhibitors or selective serotonin-norepinephrine reuptake inhibitors: American Headache Society position paper. Headache. 2010;50(6):1089-1099. (Position paper)
-
Bigal ME, Lipton RB. Excessive opioid use and the development of chronic migraine. Pain. 2009;142(3):179-182. (Review)
-
Mathew NT. Pathophysiology of chronic migraine and mode of action of preventive medications. Headache. 2011;51;Suppl 2:84-92. (Review)
-
Friedman BW, Kapoor A, Friedman MS, et al. The relative efficacy of meperidine for the treatment of acute migraine: a meta-analysis of randomized controlled trials. Ann Emerg Med. 2008;52(6):705-713. (Meta-analysis)
-
Buse DC, Pearlman SH, Reed ML, et al. Opioid use and dependence among persons with migraine: results of the AMPP study. Headache. 2012;52(1):18-36. (Survey; 5000 patients)
-
Coleman I, Rothney A, Wright SC, et al. Use of narcotic analgesics in the emergency department treatment of migraine headache. Neurology. 2004;62(10):1695-1700. (Chart review; 500 patients)
-
Tornabene SV, Deutsch R, Davis DP, et al. Evaluating the use and timing of opioids for the treatment of migraine headaches in the emergency department. J Emerg Med. 2009;36(4):333-337. (Retrospective review)
-
Innes GD, Macphail I, Dillon EC, et al. Dexamethasone prevents relapse after ED treatment of acute migraine. CJEM. 1999;1(1):26-33. (Randomized controlled trial; 98 patients)
-
Baden EY, Hunter CJ. Intravenous dexamethasone to prevent the recurrence of benign headache after discharge from the emergency department: a randomized, double-blind, placebo-controlled clinical trial. CJEM. 2006;8(6):393-400. (Randomized controlled trial; 57 patients)
-
Jones JS, Brown MD, Bermingham M, et al. Efficacy of parenteral dexamethasone to prevent relapse after ED treatment of acute migraine [abstract]. Acad Emerg Med. 2003;10:542. (Randomized controlled trial; 75 patients)
-
Fiessler FW, Shih R, Silverman ME, et al. Dexamethasone for migraine headaches: an emergency department randomized 2012double-blind placebo- controlled trial [abstract]. Acad Emerg Med. 2006;13:S137. (Randomized controlled trial; 181 patients)
-
Friedman BW, Greenwald P, Bania TC, et al. Randomized trial of IV dexamethasone for acute migraine in the emergency department. Neurology. 2007;69(22):2038-2044. (Randomized controlled trial; 205 patients)
-
Kelly AM, Kerr D, Clooney M. Impact of oral dexamethasone versus placebo after ED treatment of migraine with phenothiazines on the rate of recurrent headache: a randomized controlled trial. Emerg Med J. 2008;25(1):26-29. (Randomized controlled trial; 63 patients)
-
116. Donaldson D, Sundermann R, Jackson R, et al. Intravenous dexamethasone vs. placebo as adjunctive therapy to reduce the recurrence rate of acute migraine headaches: a multicenter, double-blinded, placebo-controlled randomized clinical trial. Am J Emerg Med. 2008;26(2):124-130. (Randomized controlled trial; 115 patients)
-
Rowe BH, Colman I, Edmonds ML, et al. Randomized controlled trial of intravenous dexamethasone to prevent relapse in acute migraine headache. Headache. 2008;48(3):333-340. (Randomized controlled trial; 130 patients)
-
Singh A, Alter HJ, Zaia B. Does the addition of dexamethasone to standard therapy for acute migraine headache decrease the incidence of recurrent headache for patients treated in the emergency department? A meta-analysis and systematic review of the literature. Acad Emerg Med. 2008;15(12):1223-1233. (Meta-analysis)
-
Colman I, Friedman BW, Brown MD, et al. Parenteral dexamethasone for acute severe migraine headache: meta-analysis of randomised controlled trials for preventing recurrence. BMJ. 2008;336(7657):1359-1361. (Meta-analysis)
-
Law S, Derry S, Moore RA. Triptans for acute cluster headache. Cochrane Database Syst Rev. 2010(4): CD008042. DOI: 10.1002/14651858.CD008042.pub2. (Meta-analysis)
-
Fogan L. Treatment of cluster headache: a double-blind comparison of oxygen v air inhalation. Arch Neurol. 1985;42(4):362-363. (Randomized controlled trial; 19 patients)
-
Cohen AS, Burns B, Goadsby PJ. High flow oxygen for treatment of cluster headache: a randomized trial. JAMA. 2009;302(22):2451-2457. (Randomized controlled trial; 109 patients)
-
Torelli P, Campana V, Cervellin G, et al. Management of primary headaches in adult emergency departments: a literature review, the Parma ED experience and a therapy flow chart proposal. Neurol Sci. 2010;31(5):545-553. (Retrospective chart review; 625 patients)
-
* Lipton RB, Stewart WF, Stone AM, et al. Stratified care vs step care strategies for migraine, the Disability in Strategies of Care (DISC) study: a randomized trial. JAMA. 2000;284(20):2599-2605. (Randomized controlled, parallel group trial; 835 patients)
-
Prensky AL, Sommer D. Diagnosis and treatment of migraine in children. Neurology. 1979;29(4):506-510.
-
Abu-Arafeh I, Razak S, Sivaraman B, et al. Prevalence of headache and migraine in children and adolescents: a systematic review of population-based studies. Dev Med Child Neurol. 2010;52(12):1088-1097. (Systematic review)
-
Rothner AD. Headaches in children and adolescents: update 2001. Semin Pediatr Neurol. 2001;8(1): 2-6. (Review)
-
Hämäläinen ML, Hoppu K, Valkeila E, et al. Ibuprofen or acetaminophen for the acute treatment of migraine in children: a double-blind, randomized, placebo-controlled, crossover study. Neurology. 1997;48(1):103–107. (Randomized controlled trial; 88 patients)
-
Lewis DW, Kellstein D, Dahl G, et al. Children’s ibuprofen suspension for the acute treatment of pediatric migraine. Headache. 2002;42(8):780-786. (Randomized controlled trial; 84 patients)
-
Soriani S, Battistella PA, Naccarella C, et al. Nimesulide and acetaminophen for the treatment of juvenile migraine: a study for comparison of efficacy, safety, and tolerability. Headache Q. 2001;12:233-236.
-
Brousseau DC, Duffy SJ, Anderson AC, Linakis JG. Treatment of pediatric migraine headaches: a randomized, double-blind trial of prochlorperazine versus ketorolac. Ann Emerg Med. 2004;43(2):256-262. (Randomized controlled trial; 62 patients)
-
Ahonen K, Hämäläinen ML, Rantala H, et al. Nasal sumatriptan is effective in treatment of migraine attacks in children: a randomized trial. Neurology. 2004;62(6):883-887. (Randomized controlled trial; 83 patients)
-
Winner P, Rothner AD, Saper J, et al. A randomized, double-blind, placebo-controlled study of sumatriptan nasal spray in the treatment of acute migraine in adolescents. Pediatrics. 2000;106(5):989-997. (Randomized controlled trial; 653 patients)
-
Ueberall MA, Wenzel D. Intranasal sumatriptan for the acute treatment of migraine in children. Neurology. 1999;52(7):1507-1510 (Randomized controlled trial; 14 patients)
-
Hämäläinen ML, Hoppu K, Santavuori P. Sumatriptan for migraine attacks in children: a randomized placebo-controlled study. Do children with migraine respond to oral sumatriptan differently from adults? Neurology. 1997;48(4):1100-1103. (Randomized controlled trial; 23 patients)
-
Somerville BW. A study of migraine in pregnancy. Neurology. 1972;22(8):824-828.
-
Ratinahirana HY, Darbois Y, Bousser M-G. Migraine and pregnancy: a prospective study in 703 women after delivery. Neurology. 1990;40:437.
-
Marcus DA, Scharff L, Turk D. Longitudinal prospective study of headache during pregnancy and postpartum. Headache. 1999;39(9):625-632. (Review)
-
Scharff L, Marcus DA, Turk DC. Headache during pregnancy and in the postpartum: a prospective study. Headache. 1997;37(4):203–210. (Prospective case series; 35 patients)
-
Pfaffenrath V, Rehm M. Migraine in pregnancy. What are the safest treatment options? Drug Saf. 1998;19(5):383-388. (Review)
-
Olesen C, Steffensen FH, Sorensen HT, et al. Pregnancy outcome following prescription for sumatriptan. Headache. 2000;40(1):20-24. (Retrospective chart review)
-
Fox AW, Chambers C, Anderson P. Evidence-based assessment of pregnancy outcome after sumatriptan exposure. Headache. 2002;42(1):8-15. (Systematic review)
-
Evans RW, Diamond ML. Is sumatriptan use safe during pregnancy? Headache. 2000;40(10):856-857. (Expert comment)
-
O’Quinn S, Ephross SA, Williams V, et al. Pregnancy and perinatal outcomes in migraineurs using sumatriptan: a prospective study. Arch Gynecol Obstet. 1999;263(1-2):7-12. (Prospective study)
-
Shuhaiber S, Pastuszak Schick B, et al. Pregnancy outcome following first trimester exposure to sumatriptan. Neurology. 1998;51(2):581–583. (Retrospective case control 96 patients)
-
Oguz KK, Yousem DM, Deluca T, et al. Effect of emergency department CT on neuroimaging case volume and positive scan rates. Acad Radiol. 2002;9(9):1018-1024. (Retrospective review)
-
FMQAI, the Support Center for the Hospital Outpatient Quality Data Reporting Program. Outpatient Imaging Efficiency Measures OP-13, OP-14 and OP-15 April 20, 2011 Webinar. http://www.hopqdrponline.com/media/OutpatientImagingEfficiencyMeasures508Checked041211_1perslide.pdf. Accessed March 25, 2012.
-
* Schurr JD, Brown MD Cheung DS, et al. Assessment of Medicare’s imaging efficiency measure for emergency department patients with atraumatic headache. Ann Emerg Med. 2012. http://www.annemergmed.com/article/S0196-0644(11)01989-5/abstract Accessed March 25, 2012. [Epub ahead of print]
-
* Friedman BW, Hochberg ML, Esses D, et al. Recurrence of primary headache disorders after emergency department discharge: frequency and predictors of poor pain and functional outcomes. Ann Emerg Med. 2008;52(6):696-704. (Prospective netcohort; 309 patients)
-
Friedman BW, Solorzano C, Esses D, et al. Treating headache recurrence after emergency department discharge: a randomized controlled trial of naproxen versus sumatriptan. Ann Emerg Med. 2010;56(1):7-17. (Randomized double blind efficacy trial; 383 patients)
-
* Swadron S. Pitfalls in the management of headache in the emergency department. Emerg Med Clin N Am. 2010;28:127-147. (Review article)
-
Matthew NT. Pathophysiology of chronic migraine and mode of action of preventive medications. Headache. 2011;51(Suppl 2):84-92. (Review article)
-
Ducharme J, Beveridge RC, Lee JS, et al. Emergency management of migraine: is the headache really over? Acad Emerg Med. 1998;5(9):899-905. (Prospective observational study; 143 patients)