Table of Contents
-
Abstract
-
Case Presentation
-
Introduction
-
Critical Appraisal Of The Literature
-
Etiology And Pathophysiology
-
Epidemiology
-
Neonatal Epidemiology
-
Differential Diagnosis
-
Neonates
-
Oral Lesions
-
Genital Lesions
-
Encephalitis
-
Prehospital Care
-
Emergency Department Evaluation
-
History
-
Neonates
-
Oral Lesions
-
Genital Lesions
-
Herpes Encephalitis
-
Physical Examination
-
Neonates
-
Oral Lesions
-
Genital Lesions
-
Herpes Encephalitis
-
Diagnostic Studies
-
Viral Culture
-
Serologic Testing
-
Polymerase Chain Reaction Testing
-
Tzanck Smear
-
Direct Fluorescent Antibody Testing
-
Lumbar Puncture
-
Liver Function Tests
-
Imaging Studies
-
Other Studies
-
Treatment
-
Neonates
-
Oral Lesions
-
Genital Lesions
-
First-Episode
-
Recurrent Episodes
-
Encephalitis
-
Vaccine
-
Special Circumstances
-
Eczema Herpeticum
-
Herpes Gladiatorum
-
Herpetic Whitlow
-
Ocular Herpes
-
Controversies And Cutting Edge
-
Disposition
-
Summary
-
Risk Management Pitfalls For Herpes Simplex Virus Infections
-
Time- And Cost-Effective Strategies
-
Case Conclusion
-
Clinical Pathway For Management Of Herpes Simplex Virus Infection In Neonates
-
Tables and Figures
-
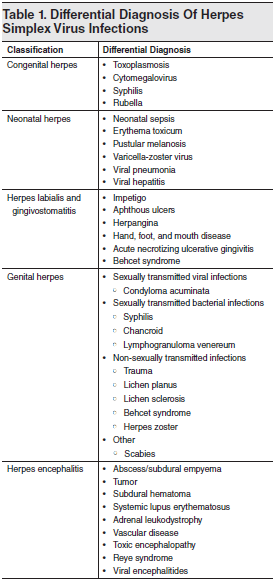
Table 1. Differential Diagnosis Of Herpes Simplex Virus Infections
-
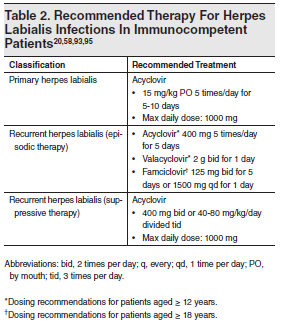
Table 2. Recommended Therapy For Herpes Labialis Infections In Immunocompetent Patients
-
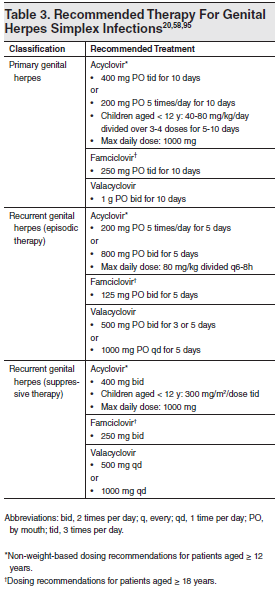
Table 3. Recommended Therapy For Genital Herpes Simplex Infections
-
Figure 1. Neonatal Herpes Simplex Virus Pustules
-
Figure 2. Herpetic Gingivostomatitis
-
Figure 3. Eczema Herpeticum
-
Figure 4. Herpetic Whitlow
-
References
Abstract
Herpes simplex virus is a common virus that causes a variety of clinical presentations ranging from mild to life-threatening. Orolabial and genital herpes are common disorders that can often be managed in an outpatient setting; however, some patients do present to the emergency department with those conditions, and emergency clinicians should be aware of possible complications in the pediatric population. Neonatal herpes is a rare disorder, but prompt recognition and initiation of antiviral therapy is imperative, as the morbidity and mortality of the disease is high. Herpes encephalitis is an emergency that also requires a high index of suspicion to diagnose. Herpes simplex virus is also responsible for a variety of other clinical presentations, including herpes gladiatorum, herpetic whitlow, eczema herpeticum, and ocular herpes. This issue reviews the common clinical presentations of the herpes simplex virus, the life-threatening infections that require expedient identification and management, and recommended treatment regimens.
Key words: herpes simplex virus, HSV1, HSV2, neonatal herpes, herpes labialis, genital herpes, herpes encephalitis, eczema herpeticum, herpes gladiatorum, herpetic whitlow, ocular herpes, polymerase chain reaction testing, Tzanck smear, lumbar puncture, liver function tests, antiviral medications, acyclovir, famciclovir, valacyclovir
Case Presentation
A 10-day-old full-term girl is brought to the ED with a rectal temperature of 38.6°C. She has no cough, congestion, runny nose, vomiting, or diarrhea. She is formulafed and is tolerating her regular feeds. The mother received prenatal care, and the prenatal labs, including Group B Streptococcus, were negative for any pathology. The mother has no reported history of HSV, but she has had a fever and throat pain for the past few days. The infant is sleeping comfortably in her mother’s arms. On examination, the anterior fontanel is soft and flat, and the skin is negative for rash or lesions. Cardiac, respiratory, and abdominal examinations are within normal limits. The infant’s temperature is now 38.7°C rectally. You explain to the medical student working with you on the case that because the baby is < 28 days old and there are no symptoms other than fever, she will require a full sepsis workup, including a lumbar puncture. You inform the medical student that this is standard of care for neonates who present with a fever, and the diagnostics will aid in determining the cause of the fever. Even though the mother has no history of HSV, you have a high index of suspicion for this. The medical student asks you if the baby should be started on acyclovir.
Introduction
Herpes simplex virus (HSV) is a common virus that affects up to 90% of the population by adulthood.1 Approximately one-third of children contract a primary HSV1 infection by the age of 5 years.2 In the United States, neonatal HSV disease occurs in approximately 1 in 3200 deliveries, or 1500 new cases annually.3 Because HSV has many clinical presentations, the emergency clinician must maintain a high index of suspicion for HSV infections and be prepared to offer the appropriate management. The emergency clinician must also be aware of possible complications in the pediatric population as well as the recommended treatments.
Critical Appraisal Of The Literature
A search was performed in PubMed for articles published since 1960 pertaining to children aged < 18 years using multiple combinations of the search terms herpes simplex virus, neonatal herpes, acyclovir, treatment, herpes encephalitis, and genital herpes. The Cochrane Database of Systematic Reviews was also consulted. Articles relevant to pediatric HSV infections were selected and reviewed. Over 300 articles were reviewed, 122 of which were chosen for inclusion in this review, including a number of randomized controlled trials, meta-analyses, and clinical practice guidelines.
Risk Management Pitfalls For Herpes Simplex Virus Infections
-
“The mother of the ill-appearing 15-day-old infant did not have a history of herpes, so the infant most likely has a bacterial infection rather than neonatal herpes.” Almost two-thirds of women who acquire genital herpes during pregnancy are asymptomatic and have no clinical findings to suggest genital HSV infection, as they have never had an HSV outbreak, nor have their partners had an outbreak.28,29,39,122
-
“The lumbar puncture was not bloody, so the patient probably does not have HSV.” While the presence of red blood cells and xanthochromia on a lumbar puncture may be seen on CSF studies in patients with HSV encephalitis or CNS involvement, 5% to 10% of patients have normal CSF studies. Red blood cells in the CSF is not a feature of neonatal infection, even with CNS involvement.27 PCR should be completed on the CSF of all patients suspected of having HSV encephalitis or CNS involvement.73 In most cases of herpes with CNS involvement, patients have either an elevated CSF white blood cell count or elevated CSF protein level, which may heighten the emergency clinician’s suspicion for CNS herpes infection.74
-
“The 3-day-old infant had pustules on the skin, so he probably has neonatal herpes.” The presence of pustules on an infant does not necessarily mean the patient has HSV. Pustular melanosis and erythema toxicum are both benign pustular eruptions that can mimic HSV.
-
“The baby was born via cesarean delivery, so herpes does not need to be ruled out.” While cesarean delivery has successfully reduced the number of neonatal herpes cases, HSV may be transmitted to an infant despite cesarean delivery.
-
“I did not see any dendrites on the fluorescein examination, so the patient does not have ocular herpes.” All patients who are suspected of having ocular herpes should be evaluated by an ophthalmologist. Findings may be subtle, and those with expertise in the evaluation of the cornea should be involved when there is any clinical concern for ocular HSV infection.
-
“The child had swelling and pain near the fingertip, so I performed an incision and drainage.” Routine incision and drainage is not recommended in patients with herpetic whitlow. Herpetic whitlow is a self-limited disease. Vesicles may be unroofed to help relieve symptoms, but deep incisions should be avoided.
-
“No lesions are visible on the external genital examination, so the patient does not have a herpes outbreak.” Patients with herpes outbreaks may not have lesions visualized on external examination. If lesions are not noted, a pelvic examination should be performed to evaluate for the presence of cervical lesions.
-
“The Tzanck prep was negative on the skin lesion of the 15-day-old infant, so HSV was ruled out.” While the Tzanck prep may be a relatively reliable test for cutaneous lesions, it does not definitively rule out neonatal herpes. If suspicion is high for neonatal herpes infection, infants require the following testing: (1) CSF for indices; (2) HSV PCR and bacterial culture; (3) viral culture swabs from the base of any vesicles as well as swabs from the mouth, conjunctiva, nasopharynx, and rectum; (4) HSV PCR on whole blood; and (5) LFTs.
-
“The CT scan on the febrile teenager with altered mental status was negative, so HSV PCR does not need to be sent on the CSF.” CT scans are less sensitive than MRI, but they may show changes (such as edema and hemorrhage) in patients with herpes encephalitis. However, early in the illness, CT and MRI may be normal, so clinical suspicion should guide management and workup.
-
“LFTs are not part of the routine sepsis rule-out. They play no role in the evaluation of febrile infants.” Elevation of serum aspartate transaminase levels > 10 times normal have been associated with increased mortality in neonates with disseminated herpes.27,32,76 Elevation of LFTs have been noted in neonates with disseminated HSV75,77 and LFT levels may serve as a screening tool for disseminated disease in those infants undergoing a sepsis rule-out.
Tables and Figures
References
Evidence-based medicine requires a critical appraisal of the literature based upon study methodology and number of subjects. Not all references are equally robust. The findings of a large, prospective, randomized, and blinded trial should carry more weight than a case report.
To help the reader judge the strength of each reference, pertinent information about the study, such as the type of study and the number of patients in the study will be included in bold type following the references, where available. The most informative references cited in this paper, as determined by the author, will be noted by an asterisk (*) next to the number of the reference.
-
Chayavichitsilp P BJ, Krakowski AC, Friedlander SF. Herpes simplex. Peds Rev. 2009;30(4):119-130. (Review)
-
Fatahzadeh M, Schwartz RA. Human herpes simplex virus infections: epidemiology, pathogenesis, symptomatology, diagnosis, and management. J Am Acad Dermatol. 2007;57(5):737-763. (Review)
-
* Brown ZA, Wald A, Morrow RA, et al. Effect of serologic status and cesarean delivery on transmission rates of herpes simplex virus from mother to infant. JAMA. 2003;289(2):203- 209. (Prospective; 58,362 patients)
-
Kimberlin DW, Rouse DJ. Clinical practice. Genital herpes. N Engl J Med. 2004;350(19):1970-1977. (Review)
-
Whitley R, Kimberlin, DW. Herpes simplex encephalitis: children and adolescents. Semin Pediatr Infect Dis. 2005;16(1):17- 23. (Review)
-
Schillinger JA, McKinney CM, Garg R, et al. Seroprevalence of herpes simplex virus type 2 and characteristics associated with undiagnosed infection: New York City, 2004. Sex Transm Dis. 2008;35(6):599-606. (Cross-sectional survey; 1999 patients)
-
Smith JS, Robinson NJ. Age-specific prevalence of infection with herpes simplex virus types 2 and 1: a global review. J Infect Dis. 2002;15(186):S3-28. (Review)
-
Xu F, Sternberg MR, Kottiri BJ, et al. Trends in herpes simplex virus type 1 and type 2 seroprevalence in the United States. JAMA. 2006;296(8):964-973. (Cross-sectional survey; 11,508 patients)
-
Fleming DT, McQuillan GM, Johnson RE, et al. Herpes simplex virus type 2 in the United States, 1976 to 1994. N Engl J Med. 1997;337(16):1105-1111. (Retrospective; 68,000 patients)
-
Armstrong GL, Schillinger J, Markowitz L, et al. Incidence of herpes simplex virus type 2 infection in the United States. Am J Epidemiol. 2001;153(9):912-920. (Cross-sectional survey; 16,691 patients)
-
Johnson RE, Nahmias AJ, Magder LS, et al. A seroepidemiologic survey of the prevalence of herpes simplex virus type 2 infection in the United States. N Engl J Med. 1989;321(1):7-12. (Retrospective; 4201 patients)
-
Nahmias AJ, Lee FK, Beckman-Nahmias S. Sero-epidemiological and -sociological patterns of herpes simplex virus infection in the world. Scand J Infect Dis Suppl. 1990;69:19-36. (Retrospective; 40,000 patients)
-
Ribes JA, Steele, AD, Seabolt, JP, et al. Six-year study of the incidence of herpes in genital and nongenital cultures in a central Kentucky medical center patient population. J Clin Microbiol. 2001;39(9):3321-3325. (Retrospective; 4595 patients)
-
Scoular AL, Leask BG, Carrington D. Changing trends in genital herpes due to herpes simplex virus type 1 in Glasgow, 1985-88. Genitourin Med. 1990;66(3):226. (Letter to the editor)
-
Nilsen A, Myrmel, H. Changing trends in genital herpes simplex virus infection in Bergen, Norway. Acta Obstet Gynecol Scand. 2000;79(8):693-696. (Retrospective; 1023 patients)
-
Tayal SCP, R.S High prevalence of herpes simplex virus type 1 in female anogenital herpes simplex in Newcastle upon Tyne 1983-92. Int J STD AIDS. 1994;5(5):359-361. (Retrospective; 1135 patients)
-
Roberts CM, Pfister JR, Spear SJ. Increasing proportion of herpes simplex virus type 1 as a cause of genital herpes infection in college students. Sex Transm Dis. 2003;30(10):797- 800. (Retrospective; 499 patients)
-
Schillinger JA, Xu F, Sternberg MR, et al. National seroprevalence and trends in herpes simplex virus type 1 in the United States, 1976-1994. Sex Transm Dis. 2004;31(12):753-760. (Cross-sectional survey; 27,801 patients)
-
Anderson WE. Herpes Simplex Encephalitis. 2013; Available at http://emedicine.medscape.com/article/1165183-overview. Accessed August 2, 2013. (Review)
-
Whitley RJ, Soong SJ, Linneman C, Jr, et al. Herpes simplex encephalitis. Clinical assessment. JAMA. 1982;247(3):317-320. (Review)
-
James SH, Whitley RJ. Treatment of herpes simplex virus infections in pediatric patients: current status and future needs. Clin Pharmacol Ther. 2010;88(5):720-724. (Review)
-
Whitley R. Herpes simplex encephalitis: adolescents and adults. Antiviral Res. 2006;71(2-3):141-148. (Review)
-
Whitley R, Davis EA, Suppapanya N. Incidence of neonatal herpes simplex virus infections in a managed-care population. Sex Transm Dis. 2007;34(9):704-708. (Retrospective; 566 patients)
-
Marquez L, Levy ML, Munoz FM, et al. A report of three cases and review of intrauterine herpes simplex virus infection. Pediatr Infect Dis J. 2011;30(2):153-157. (Retrospective; 64 patients)
-
Whitley R, Arvin A, Prober C, et al. Predictors of morbidity and mortality in neonates with herpes simplex virus infections. The National Institute of Allergy and Infectious Diseases Collaborative Antiviral Study Group. N Engl J Med. 1991;324(7):450-454. (Prospective; 202 patients)
-
Whitley R, Arvin A, Prober C, et al. A controlled trial comparing vidarabine with acyclovir in neonatal herpes simplex virus infection. Infectious Diseases Collaborative Antiviral Study Group. N Engl J Med. 1991;324(7):444-449. (Prospective; 202 patients)
-
Kimberlin DW, Lin CY, Jacobs RF, et al. Natural history of neonatal herpes simplex virus infections in the acyclovir era. Pediatrics. 2001;108(2):223-229. (Prospective; 186 patients)
-
Whitley RJ, Nahmias AJ, Visintine AM, et al. The natural history of herpes simplex virus infection of mother and newborn. Pediatrics. 1980;66(4):489-494. (Retrospective; 56 patients)
-
Whitley RJ, Corey L, Arvin A, et al. Changing presentation of herpes simplex virus infection in neonates. J Infect Dis. 1988;158(1):109-116. (Retrospective; 291 patients)
-
* Kimberlin DW, Lin CY, Jacobs RF, et al. Safety and efficacy of high-dose intravenous acyclovir in the management of neonatal herpes simplex virus infections. Pediatrics. 2001;108(2):230-238. (Prospective and retrospective; 195 patients)
-
Whitley RJ, Nahmias AJ, Soong SJ, et al. Vidarabine therapy of neonatal herpes simplex virus infection. Pediatrics. 1980;66(4):495-501. (Prospective; 56 patients)
-
Kimberlin D. Herpes simplex virus, meningitis and encephalitis in neonates. Herpes. 2004;11 Suppl 2:65A-76A. (Review)
-
Zitelli BJ, Davis HW. Atlas of Pediatric Physical Diagnosis. 4th ed. St. Louis, MO: Mosby Inc; 2002:396-454. (Textbook)
-
Kimberlin DW. Herpes simplex virus infections of the newborn. Semin Perinatol. 2007;31(1):19-25. (Review)
-
* Kimberlin DW, Baley J. Guidance on management of asymptomatic neonates born to women with active genital herpes lesions. Pediatrics. 2013;131(2):383-386. (Clinical practice guidelines)
-
* Brown ZA, Benedetti J, Ashley R, et al. Neonatal herpes simplex virus infection in relation to asymptomatic maternal infection at the time of labor. N Engl J Med. 1991;324(18):1247- 1252. (Prospective; 15,923 patients)
-
Brown ZA, Vontver LA, Benedetti J, et al. Effects on infants of a first episode of genital herpes during pregnancy. N Engl J Med. 1987;317(20):1246-1251. (Prospective; 29 patients)
-
Prober CG, Sullender WM, Yasukawa LL, et al. Low risk of herpes simplex virus infections in neonates exposed to the virus at the time of vaginal delivery to mothers with recurrent genital herpes simplex virus infections. N Engl J Med. 1987;316(5):240-244. (Retrospective; 34 patients)
-
Yeager AS, Arvin AM, Urbani LJ, et al. Relationship of antibody to outcome in neonatal herpes simplex virus infections. Infect Immun. 1980;29(2):532-538. (Prospective; 166 patients)
-
Kaye EM, Dooling EC. Neonatal herpes simplex meningoencephalitis associated with fetal monitor scalp electrodes. Neurology. 1981;31(8):1045-1047. (Retrospective; 2 patients)
-
Parvey LS, Ch’ien LT. Neonatal herpes simplex virus infection introduced by fetal-monitor scalp electrodes. Pediatrics. 1980;65(6):1150-1153. (Retrospective; 1 patient)
-
* ACOG practice bulletin. Management of herpes in pregnancy. Number 8 October 1999. Clinical management guidelines for obstetrician-gynecologists. Int J Gynaecol Obstet. 2000;68(2):165- 173. (Clinical practice guidelines)
-
Randolph AG, Hartshorn RM, Washington AE. Acyclovir prophylaxis in late pregnancy to prevent neonatal herpes: a cost-effectiveness analysis. Obstet Gynecol. 1996;88(4 Pt 1):603-610. (Cost-effectiveness analysis)
-
Brocklehurst P, Kinghorn G, Carney O, et al. A randomised placebo-controlled trial of suppressive acyclovir in late pregnancy in women with recurrent genital herpes infection. Br J Obstet Gynaecol. 1998;105(3):275-280. (Prospective; 63 patients)
-
Braig S, Luton D, Sibony O, et al. Acyclovir prophylaxis in late pregnancy prevents recurrent genital herpes and viral shedding. Eur J Obstet Gynecol Reprod Biol. 2001;96(1):55-58. (Prospective; 288 patients)
-
* Hollier LM, Wendel GD. Third trimester antiviral prophylaxis for preventing maternal genital herpes simplex virus (HSV) recurrences and neonatal infection. Cochrane Database Syst Rev. 2008;23(1). (Meta-analysis; 7 trials, 1249 patients)
-
Scott LL, Hollier LM, McIntire D, et al. Acyclovir suppression to prevent recurrent genital herpes at delivery. Infect Dis Obstet Gynecol. 2002;10(2):71-77. (Prospective; 234 patients)
-
Scott LL, Hollier LM, McIntire D, et al. Acyclovir suppression to prevent clinical recurrences at delivery after first episode genital herpes in pregnancy: an open-label trial. Infect Dis Obstet Gynecol. 2001;9(2):75-80. (Prospective; 96 patients)
-
Scott LL, Sanchez PJ, Jackson GL, et al. Acyclovir suppression to prevent cesarean delivery after first-episode genital herpes. Obstet Gynecol. 1996;87(1):69-73. (Prospective; 46 patients)
-
* Watts DH, Brown ZA, Money D, et al. A double-blind, randomized, placebo-controlled trial of acyclovir in late pregnancy for the reduction of herpes simplex virus shedding and cesarean delivery. Am J Obstet Gynecol. 2003;188(3):836- 843. (Prospective; 162 patients)
-
* Sheffield JS, Hill JB, Hollier LM, et al. Valacyclovir prophylaxis to prevent recurrent herpes at delivery: a randomized clinical trial. Obstet Gynecol. 2006;108(1):141-147. (Prospective; 350 patients)
-
Pinninti SG, Angara R, Feja KN, et al. Neonatal herpes disease following maternal antenatal antiviral suppressive therapy: a multicenter case series. J Pediatr. 2012;161(1):134- 138. (Case series; 8 patients)
-
Baldwin S, Whitley RJ. Intrauterine herpes simplex virus infection. Teratology. 1989;39(1):1-10. (Review)
-
Johansson AB, Rassart A, Blum D, et al. Lower-limb hypoplasia due to intrauterine infection with herpes simplex virus type 2: possible confusion with intrauterine varicella-zoster syndrome. Clin Infect Dis. 2004;38(7):e57-e62. (Retrospective; 1 patient)
-
Arvin AM, Yeager AS, Bruhn FW, et al. Neonatal herpes simplex infection in the absence of mucocutaneous lesions. J Pediatr. 1982;100(5):715-721. (Retrospective; 20 patients)
-
Corey L, Adams HG, Brown ZA, et al. Genital herpes simplex virus infections: clinical manifestations, course, and complications. Ann Intern Med. 1983;98(6):958-972. (Review)
-
Glass N, Nelson HD, Huffman, L. U.S. Preventive Services Task Force. Screening for genital herpes: recommendation statement. Am Fam Phys. 2005;72(8):1557-1561. (Recommendation statement)
-
Pickering L, Baker C, Kimberlin D. Herpes Simplex. American Academy of Pediatrics. Red Book: 2012 Report of the Committee on Infectious Diseases. Pickering LK, ed. 29th ed. Elk Grove Village, IL: American Academy of Pediatrics; 2012:398-408. (Report)
-
Singh A, Preiksaitis J, Ferenczy A, et al. The laboratory diagnosis of herpes simplex virus infections. Can J Infect Dis Med Microbiol. 2005;16(2):92-98. (Review)
-
Ashley RL, Wald A, Eagleton M. Premarket evaluation of the POCkit HSV-2 type-specific serologic test in culturedocumented cases of genital herpes simplex virus type 2. Sex Transm Dis. 2000;27(5):266-269. (Prospective; 303 patients)
-
Ashley RL, Eagleton M. Evaluation of a novel point of care test for antibodies to herpes simplex virus type 2. Sex Transm Infect. 1998;74(3):228-229. (Review)
-
Leach CT, Ashley RL, Baillargeon J, et al. Performance of two commercial glycoprotein G-based enzyme immunoassays for detecting antibodies to herpes simplex viruses 1 and 2 in children and young adolescents. Clin Diagn Lab Immunol. 2002;9(5):1124-1125. (Retrospective; 61 patients)
-
Ashley RL. Performance and use of HSV type-specific serology test kits. Herpes. 2002;9(1):38-45. (Review)
-
Scoular A. Using the evidence base on genital herpes: optimising the use of diagnostic tests and information provision. Sex Transm Infect. 2002;78(3):160-165. (Review)
-
Irani DN, Greenberg BM. Cerebrospinal Fluid in Clinical Practice. 1st ed. Philadelphia PA: Saunders; 2009:177-190. (Review)
-
Kimberlin DW, Lakeman FD, Arvin AM, et al. Application of the polymerase chain reaction to the diagnosis and management of neonatal herpes simplex virus disease. National Institute of Allergy and Infectious Diseases Collaborative Antiviral Study Group. J Infect Dis. 1996;174(6):1162-1167. (Retrospective; 77 patients)
-
Troendle-Atkins J, Demmler GJ, Buffone GJ. Rapid diagnosis of herpes simplex virus encephalitis by using the polymerase chain reaction. J Pediatr. 1993;123(3):376-380. (Prospective; 124 patients)
-
Kimura H, Futamura M, Kito H, et al. Detection of viral DNA in neonatal herpes simplex virus infections: frequent and prolonged presence in serum and cerebrospinal fluid. J Infect Dis. 1991;164(2):289-293. (Prospective; 7 patients)
-
Lakeman FD, Whitley RJ. Diagnosis of herpes simplex encephalitis: application of polymerase chain reaction to cerebrospinal fluid from brain-biopsied patients and correlation with disease. National Institute of Allergy and Infectious Disease Collaborative Antiviral Study Group. J Infect Dis. 1995;171(4):857-863. (Retrospective; 101 patients)
-
Atkins JT. HSV PCR for CNS infections: pearls and pitfalls. Pediatr Infect Dis J. 1999;18(9):823-824. (Review)
-
Ozcan A, Senol M, Saglam H, et al. Comparison of the Tzanck test and polymerase chain reaction in the diagnosis of cutaneous herpes simplex and varicella zoster virus infections. Int J Dermatol. 2007;46(11):1177-1179. (Retrospective; 98 patients)
-
Caviness AC, Oelze LL, Saz UE, et al. Direct immunofluorescence assay compared to cell culture for the diagnosis of mucocutaneous herpes simplex virus infections in children. J Clin Virol. 2010;49(1):58-60. (Retrospective; 659 patients)
-
Mook-Kanamori B, van de Beek D, Wijdicks EF. Herpes simplex encephalitis with normal initial cerebrospinal fluid examination. J Am Geriatr Soc. 2009;57(8):1514-1515. (Retrospective; 1 patient)
-
Hanson KE, Alexander BD, Woods C, et al. Validation of laboratory screening criteria for herpes simplex virus testing of cerebrospinal fluid. J Clin Microbiol. 2007;45(3):721- 724. (Retrospective; 1458 patients)
-
* Caviness AC, Demmler GJ, Almendarez Y, et al. The prevalence of neonatal herpes simplex virus infection compared with serious bacterial illness in hospitalized neonates. J Pediatr. 2008;153(2):164-169. (Retrospective; 5817 patients)
-
Fidler KJ, Pierce CM, Cubitt WD, et al. Could neonatal disseminated herpes simplex virus infections be treated earlier? J Infect. 2004;49(2):141-146. (Retrospective; 8 patients)
-
Caviness AC, Demmler GJ, Selwyn BJ. Clinical and laboratory features of neonatal herpes simplex virus infection: a case-control study. Pediatr Infect Dis J. 2008;27(5):425-430. (Case-control; 200 patients)
-
Tunkel AR, Glaser CA, Bloch KC, et al. The management of encephalitis: clinical practice guidelines by the Infectious Diseases Society of America. Clin Infect Dis. 2008;47(3):303- 327. (Clinical practice guidelines)
-
Gasecki AP, Steg RE. Correlation of early MRI with CT scan, EEG, and CSF: analyses in a case of biopsy-proven herpes simplex encephalitis. Eur Neurol. 1991;31(6):372-375. (Case study; 1 patient)
-
Go RT, Yousef MM, Jacoby CG. The role of radionuclide brain imaging and computerized tomography in the early diagnosis of herpes simplex encephalitis. J Comput Tomogr. 1979;3(4):286-296. (Retrospective; 12 patients)
-
Goldstein MA, Harden CL. Herpes encephalitis. Available at http://professionals.epilepsy.com/page/viral_herp_enceph. html. Accessed August 7, 2013. (Review)
-
Toth C, Harder S, Yager J. Neonatal herpes encephalitis: a case series and review of clinical presentation. Can J Neurol Sci. 2003;30(1):36-40. (Case series; 9 patients)
-
Whitley RJ, Alford CA, Hirsch MS, et al. Vidarabine versus acyclovir therapy in herpes simplex encephalitis. N Engl J Med. 1986;314(3):144-149. (Prospective; 208 patients)
-
Englund JA FC, Balfour HH. Acyclovir therapy in neonates. J Pediatr. 1991(119):129-135. (Prospective; 16 patients)
-
Long SS. In defense of empiric acyclovir therapy in certain neonates. J Pediatr. 2008;153(2):157-158. (Editorial)
-
Annunziato PW, Gershon A. Herpes simplex virus infections. Pediatr Rev. 1996;17(12):415-423. (Review)
-
Shah SS, Aronson PL, Mohamad Z, et al. Delayed acyclovir therapy and death among neonates with herpes simplex virus infection. Pediatrics. 2011;128(6):1153-1160. (Retrospective; 1086 patients)
-
Long SS, Pool TE, Vodzak J, et al. Herpes simplex virus infection in young infants during 2 decades of empiric acyclovir therapy. Pediatr Infect Dis J. 2011;30(7):556-561. (Retrospective; 32 patients)
-
Kimberlin DW, Whitley RJ, Wan W, et al. Oral acyclovir suppression and neurodevelopment after neonatal herpes. N Engl J Med. 2011;365(14):1284-1292. (Prospective; 74 patients)
-
Kimberlin D, Powell D, Gruber W, et al. Administration of oral acyclovir suppressive therapy after neonatal herpes simplex virus disease limited to the skin, eyes and mouth: results of a phase I/II trial. Pediatr Infect Dis J. 1996;15(3):247- 254. (Prospective; 26 patients)
-
Rudd C, Rivadeneira ED, Gutman LT. Dosing considerations for oral acyclovir following neonatal herpes disease. Acta Paediatr. 1994;83(12):1237-1243. (Retrospective; 9 patients)
-
* Nasser M, Fedorowicz Z, Khoshnevisan MH, et al. Acyclovir for treating primary herpetic gingivostomatitis. Cochrane Database Syst Rev. 2008(4):CD006700. (Meta-analysis; 2 trials, 92 patients)
-
Nikkels AF, Pièrard GE. Treatment of mucocutaneous presentations of herpes simplex virus infections. Am J Clin Dermatol. 2002;3(7):475-487. (Review)
-
Brady RC, Bernstein DI. Treatment of herpes simplex virus infections. Antiviral Res. 2004;61(2):73-81. (Review)
-
Cernik C, Gallina K, Brodell RT. The treatment of herpes simplex infections: an evidence-based review. Arch Intern Med. 2008;168(11):1137-1144. (Review)
-
Mertz GJ, Jones CC, Mills J, et al. Long-term acyclovir suppression of frequently recurring genital herpes simplex virus infection. A multicenter double-blind trial. JAMA. 1988;260(2):201-206. (Prospective; 1146 patients)
-
Fife KH, Crumpacker CS, Mertz GJ, et al. Recurrence and resistance patterns of herpes simplex virus following cessation of > or=6 years of chronic suppression with acyclovir. Acyclovir Study Group. J Infect Dis. 1994;169(6):1338-1341. (Prospective; 243 patients)
-
Goldberg LH, Kaufman R, Kurtz TO, et al. Long-term suppression of recurrent genital herpes with acyclovir. A 5-year benchmark. Acyclovir Study Group. Arch Dermatol. 1993;129(5):582-587. (Prospective; 1146 patients)
-
Stanberry LR, Spruance SL, Cunningham AL, et al. Glycoprotein- D-adjuvant vaccine to prevent genital herpes. N Engl J Med. 2002;347(21):1652-1661. (Prospective; 243 patients)
-
Belshe RB, Leone PA, Bernstein DI, et al. Efficacy results of a trial of a herpes simplex vaccine. N Engl J Med. 2012;366(1):34-43. (Prospective; 8323 patients)
-
Wheeler C AD. Eczema herpeticum, primary and recurrent. Arch Dermat. 1966;93:162-173. (Retrospective; 2 patients)
-
Terezhalmy GT, Tyler MT, Ross GR. Eczema herpeticum: atopic dermatitis complicated by primary herpetic gingivostomatitis. Oral Surg Oral Med Oral Pathol. 1979;48(6):513-516. (Case report; 1 patient)
-
Luca NJ, Lara-Corrales I, Pope E. Eczema herpeticum in children: clinical features and factors predictive of hospitalization. J Pediatr. 2012;161(4):671-675. (Retrospective; 79 patients)
-
Atherton DJ, Marshall WC. Eczema herpeticum. Practitioner. 1982;226(1367):971-973. (Review)
-
Liaw FY, Huang CF, Hsueh JT, et al. Eczema herpeticum. Can Fam Physician. 2012;58:1358-1361. (Case study; 1 patient)
-
Mackley CL, Adams DR, Anderson B, et al. Eczema herpeticum: a dermatologic emergency. Derm Nurs. 2002;14(5):307- 310. (Review)
-
Aronson PL, Yan AC, Mohamad Z, et al. Empiric antibiotics and outcomes of children hospitalized with eczema herpeticum. Pediatr Dermatol. 2013;30(2):207-214. (Retrospective; 1150 patients)
-
Aronson PL, Shah SS, Mohamad Z, et al. Topical corticosteroids and hospital length of stay in children with eczema herpeticum. Pediatr Dermatol. 2013;30(2):215-221. (Retrospective; 1331 patients)
-
Selling B, Kibrick S. An outbreak of herpes simplex among wrestlers (herpes gladiatorum). N Engl J Med. 1964;270:979- 982. (Retrospective; 6 patients)
-
Likness LP. Common dermatologic infections in athletes and return-to-play guidelines. J Am Osteo Ass. 2011;111(6):373- 379. (Review)
-
Anderson BJ. Managing herpes gladiatorum outbreaks in competitive wrestling: the 2007 Minnesota experience. Curr Sports Med Rep. 2008;7(6):323-327. (Review)
-
National Federation of State High School Associations SMAC. Sports-related skin infections position statement and guidelines. 2013. Available at: http://www.mshsaa.org/ resources/ pdf/2013%2020Skin.pdf. Accessed July 20, 2013. (Clinical practice guidelines)
-
Anderson BJ. Prophylactic valacyclovir to prevent outbreaks of primary herpes gladiatorum at a 28-day wrestling camp. Jpn J Infect Dis. 2006;59(1):6-9. (Prospective; 94 patients)
-
Gill MJ, Arlette J, Buchan K. Herpes simplex virus infection of the hand. A profile of 79 cases. Am J Med. 1988;84(1):89-93. (Retrospective; 79 patients)
-
Feder HM Jr, Long SS. Herpetic whitlow. Epidemiology, clinical characteristics, diagnosis, and treatment. Am J Dis Child. 1983;137(9):861-863. (Case series; 8 patients)
-
Wilhelmus KR. Antiviral treatment and other therapeutic interventions for herpes simplex virus epithelial keratitis. Cochrane Database Syst Rev. 2010(12): CD002898. (Meta-analysis; 106 trials, 5872 eyes)
-
Collum LM, McGettrick P, Akhtar J, et al. Oral acyclovir (Zovirax) in herpes simplex dendritic corneal ulceration. Br J Ophthalmol. 1986;70(6):435-438. (Prospective; 60 patients)
-
Distel R, Hofer V, Bogger-Goren S, et al. Primary genital herpes simplex infection associated with Jewish ritual circumcision. Isr Med Assoc J. 2003;5(12):893-894. (Case study; 1 patient)
-
Rubin LG, Lanzkowsky P. Cutaneous neonatal herpes simplex infection associated with ritual circumcision. Pediatr Infect Dis J. 2000;19(3):266-268. (Case studies; 2 patients)
-
Gesundheit B, Grisaru-Soen G, Greenberg D, et al. Neonatal genital herpes simplex virus type 1 infection after Jewish ritual circumcision: modern medicine and religious tradition. Pediatrics. 2004;114(2):e259-e263. (Retrospective; 8 patients)
-
Neonatal herpes simplex virus infection following Jewish ritual circumcisions that included direct orogenital suction - New York City, 2000-2011. MMWR Morb Mortal Wkly Rep. 2012;61(22):405-409. (Retrospective; 11 patients)
-
Brown ZA, Selke S, Zeh J, et al. The acquisition of herpes simplex virus during pregnancy. N Engl J Med. 1997;337(8):509-515. (Retrospective; 7046 patients)