
|
|
Wide complex tachycardia encompasses a range of cardiac tachydysrhythmias, several of which can be life-threatening, difficult to distinguish, and require distinct treatment approaches. This review summarizes the etiologies and pathophysiology of wide complex tachycardia, outlines the differential diagnosis, and provides an evidence-based approach to distinguishing the various types using the history, physical examination, electrocardiography, and response to intravenous adenosine. Management strategies and disposition decisions are also reviewed, with attention to special clinical circumstances and selected areas of ongoing controversy, including emerging artificial intelligence tools.
How would you manage these patients? Subscribe for evidence-based best practices and to discover the outcomes.
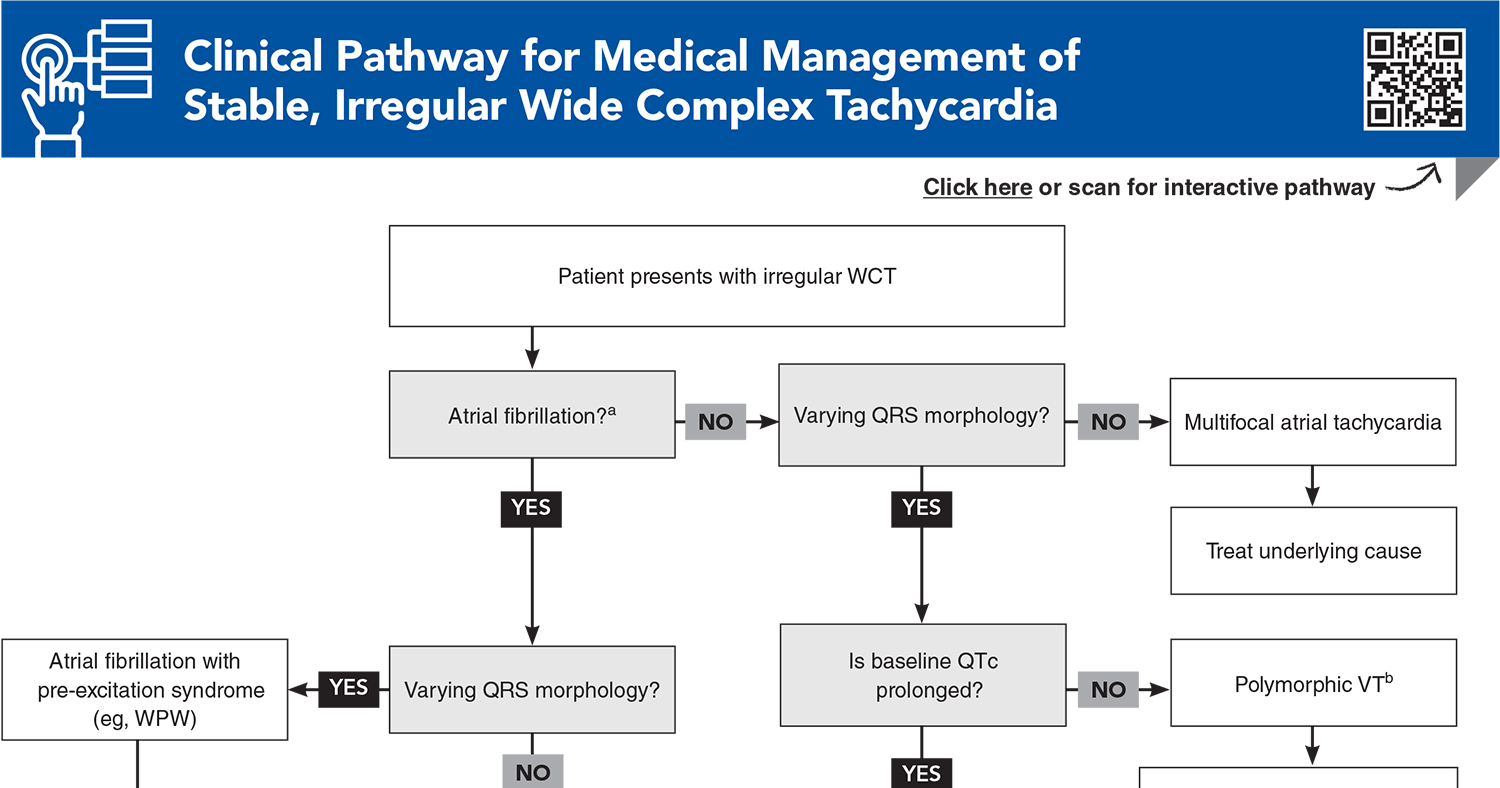
Subscribe to access the complete Clinical Pathway to guide your clinical decision making.
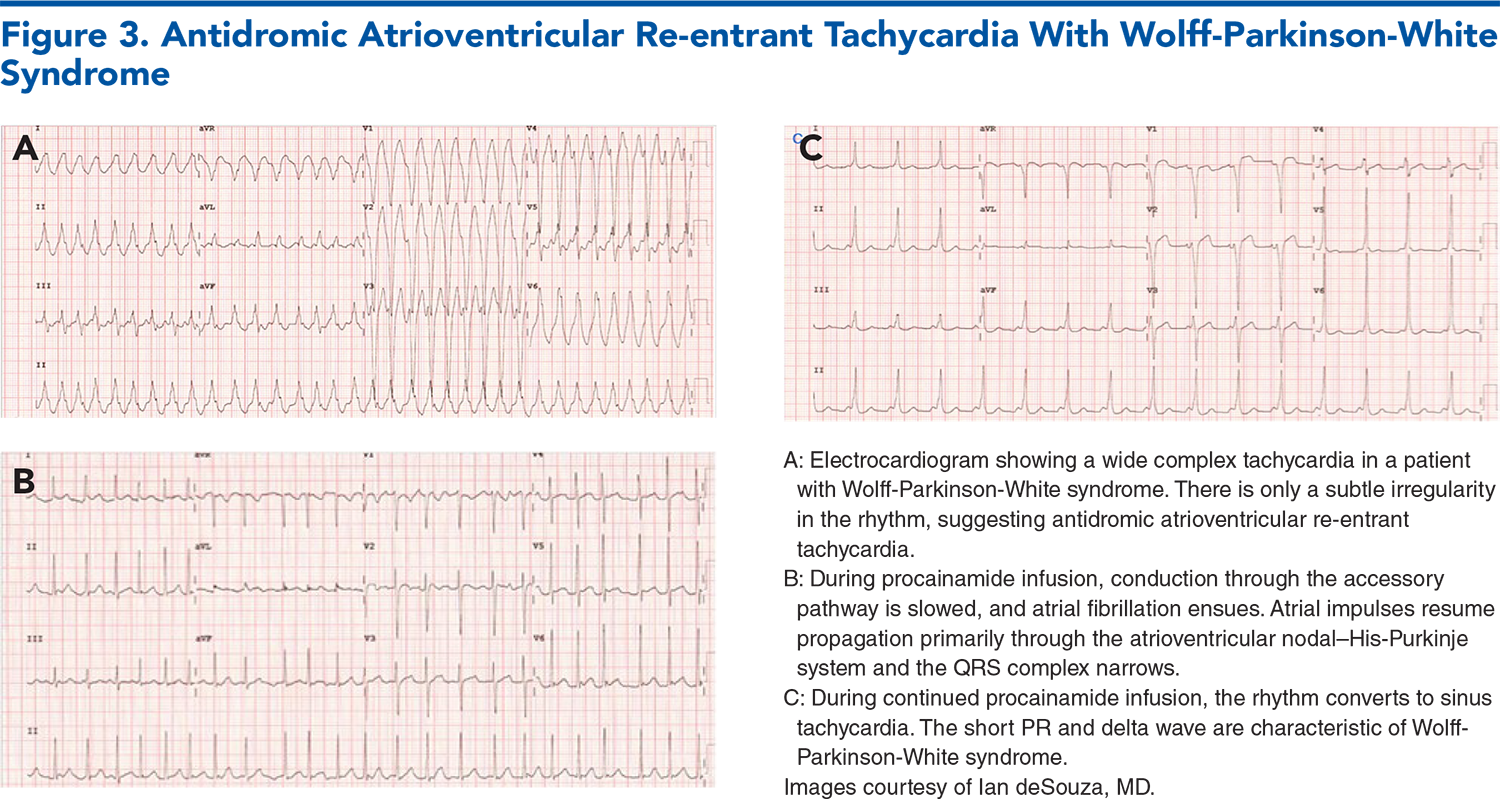
Subscribe for full access to all Tables and Figures.
Buy this issue and
Following are the most informative references cited in this paper, as determined by the authors.
9. * Wigginton JG, Agarwal S, Bartos JA, et al. Part 9: adult advanced life support: 2025 American Heart Association guidelines for cardiopulmonary resuscitation and emergency cardiovascular care. Circulation. 2025;152(16_suppl_2):S538-S577. (Clinical practice guidelines) DOI: 10.1161/CIR.0000000000001376
20. * Alblaihed L, Al-Salamah T. Wide complex tachycardias. Emerg Med Clin North Am. 2022;40(4):733-753. (Review) DOI: 10.1016/j.emc.2022.06.010
28. * Brady WJ, Mattu A, Tabas J, et al. The differential diagnosis of wide QRS complex tachycardia. Am J Emerg Med. 2017;35(10):1525-1529. (Review) DOI: 10.1016/j.ajem.2017.07.056
40. * Marill KA, Wolfram S, deSouza IS, et al. Adenosine for wide-complex tachycardia: efficacy and safety. Crit Care Med. 2009;37(9):2512-2518. (Retrospective; 197 patients) DOI: 10.1097/CCM.0b013e3181a93661
61. * Kashou AH, Noseworthy PA, DeSimone CV, et al. Wide complex tachycardia differentiation: a reappraisal of the state-of-the-art. J Am Heart Assoc. 2020;9(11):e016598. (Review) DOI: 10.1161/JAHA.120.016598
63. * Al-Khatib SM, Stevenson WG, Ackerman MJ, et al. 2017 AHA/ACC/HRS guideline for management of patients with ventricular arrhythmias and the prevention of sudden cardiac death: executive summary: a report of the American College of Cardiology/American Heart Association task force on clinical practice guidelines and the Heart Rhythm Society. Circulation. 2018;138(13):e210-e271. (Clinical practice guideline) DOI: 10.1161/CIR.0000000000000548
84. * Zeppenfeld K, Tfelt-Hansen J, de Riva M, et al. 2022 ESC guidelines for the management of patients with ventricular arrhythmias and the prevention of sudden cardiac death. Eur Heart J. 2022;43(40):3997-4126. (Clinical practice guidelines) DOI: 10.1093/eurheartj/ehac262
86. * Ortiz M, Martin A, Arribas F, et al. Randomized comparison of intravenous procainamide vs. intravenous amiodarone for the acute treatment of tolerated wide QRS tachycardia: the PROCAMIO study. Eur Heart J. 2017;38(17):1329-1335. (Randomized controlled trial; 74 patients) DOI: 10.1093/eurheartj/ehw230
94. * Cao D, Arens AM, Chow SL, et al. Part 10: adult and pediatric special circumstances of resuscitation: 2025 American Heart Association guidelines for cardiopulmonary resuscitation and emergency cardiovascular care. Circulation. 2025;152(16_suppl_2):S578-S672. (Clinical practice guidelines) DOI: 10.1161/CIR.0000000000001380
Subscribe to get the full list of 112 references and see how the authors distilled all of the evidence into a concise, clinically relevant, practical resource.
Keywords: wide complex tachycardia, ECG, EKG, ventricular tachycardia, wide QRS tachycardia, supraventricular tachycardia, VT, SVT, tachydysrhythmia, tachyarrhythmia, stable WCT, unstable WCT, adenosine, procainamide, amiodarone, Wolff-Parkinson-White, Brugada, Wells, atrial fibrillation, atrial flutter
Robert Allen, MD; Caleb J. Bailie, MD; Ian S. deSouza, MD
April 1, 2026
April 1, 2029 CME Information
4 AMA PRA Category 1 Credits™, 4 ACEP Category I Credits, 4 AAFP Prescribed Credits, 4 AOA Category 2-B Credits. Specialty CME Credits: Included as part of the 4 credits, this CME activity is eligible for 2 Pharmacology CME credits, subject to your state and institutional approval.