Table of Contents
About This Issue
Most marine life injuries are non─life-threatening, and patients who present to urgent care are typically clinically stable, but these injuries carry important risks including infection, retained foreign bodies, tissue necrosis, and, in rare cases, delayed systemic toxicity. Urgent care clinicians play an important role in these types of injuries, as they are often the first healthcare professionals to evaluate these patients. Management should focus on mechanism of injury (puncture, sting, laceration), depth of penetration, and presence of systemic symptoms rather than species identification or wound size. Core treatment principles include prompt pain control, copious irrigation with antiseptic solution, removal of accessible foreign material, tetanus review, and risk-based antibiotic decisions. Clear criteria for referral to specialty care is included. In this issue, you will learn:
How to evaluate patients presenting to urgent care with marine envenomation or injury using a systematic approach based on mechanism, severity, and timing of symptoms;
That dangerous local marine organisms may cause injury and understand how geography influences risk;
The importance of being familiar with local venomous marine life and recognizing the complications of their exposure; and
How to determine evidence-based treatment strategies, including pain control, wound management, antibiotic use, and criteria for referral.
CODING & CHARTING: Accurately detailing your clinical notes will support the level of care provided for patients presenting to urgent care with common marine life injuries or envenomations. Learn more in our monthly coding column.
- About This Issue
- Abstract
- Case Presentations
- Introduction
- Etiology and Pathophysiology
- Overview of Organisms
- Jellyfish (Phylum Cnidaria)
- Siphonophores
- Box Jellyfish
- Irukandji Jellyfish
- Sea Urchins (Phylum Echinodermata)
- Crown-of-Thorns Starfish
- Flower Urchin
- Venomous Fish (Family Scorpaenidae)
- Stingrays (Class Chondrichthyes)
- Octopods (Class Cephalopoda)
- Sea Snakes/Sea Kraits (Family Elapidae)
- Cone Snails (Family Conoidea)
- Fire Coral (Genus Millepora)
- Larval and Cercaria Skin Irritations
- Swimmer’s Itch
- Seabather’s Eruption
- Differential Diagnosis
- Urgent Care Evaluation
- History
- Physical Examination
- Diagnostic Studies
- Treatment
- General Management
- Pain Management
- Removal of Foreign Bodies
- Decontamination and Infection Control
- Monitoring Systemic Symptoms
- Recommendations for Specific Marine Organism Injuries
- Jellyfish
- Box Jellyfish
- Other Jellyfish
- Sea Urchins
- Venomous Fish
- Stingrays
- Blue-Ringed Octopods
- Sea Snakes/Sea Kraits
- Cone Snails
- Fire Coral
- Swimmer’s Itch and Seabather’s Eruption
- Swimmer’s Itch
- Seabather’s Eruption
- Antibiotic Treatment and Prophylaxis
- Disposition
- Special Populations
- Patients With Heart Disease
- Patients With Chronic Disease
- Patients With Atopic History
- Controversies
- Use of Vinegar
- Use of Urine
- Other Remedies
- Summary
- Critical Appraisal of the Literature
- Time and Cost-Effective Strategies
- 5 Things That Will Change Your Practice
- Risk Management Pitfalls for Urgent Care Management of Marine Life Injuries and Envenomations
- Case Conclusions
- Coding & Charting: What You Need to Know
- Coding Challenge: Presentation of Marine Injury in Urgent Care
- Clinical Pathway for Urgent Care Management of Patients With Marine Life Injuries and Envenomations
- References
Abstract
Most presentations of marine life injuries and envenomations to the urgent care setting are non–life-threatening; they may include infections, retention of foreign material, systemic allergy symptoms, and skin irritation. However, patients may present with a wide spectrum of animal encounters, time since injury, and illness severity. Little has changed over the past 20 years related to marine life injuries and associated wound care, apart from first-aid guidelines for jellyfish stings, with an emphasis on the most lethal species. Because urgent care clinicians are often the first healthcare professionals to evaluate these patients, they play a pivotal role in early intervention, risk stratification, and timely escalation of care, when indicated. This issue of Evidence-Based Urgent Care provides practical guidance on the recognition, initial assessment, and management of marine life injuries, including recommendations for clinic-based treatment and clear criteria for referral to higher levels of care.
Case Presentations
- He was playing in the surf on a North Carolina beach with his friends when he saw a jellyfish wrapped around his left leg and foot.
- A bystander saw what happened and helped the boy wash off his legs and feet in saltwater.
- His left leg and foot are red and inflamed.
- On physical examination, he has no systemic symptoms but does have local erythema and itching.
- You wonder what kind of jellyfish may have stung him…
- He reports that he was climbing over a rocky intertidal area, when he slipped and fell into the water. The patient was punctured by multiple sea urchin spines in his right ankle and Achilles tendon.
- You wonder if he needs urgent referral for surgical evaluation ...
- Two days ago, she was scuba diving for invasive lionfish. She speared one, but punctured her right index finger with its spine while trying to remove it from her spear. She had immediate pain.
- She washed the finger thoroughly with chlorhexidine and water, and then soaked her finger in hot water, which helped the pain.
- She applied ice after she continued to have pain and swelling.
- Two days after the injury, is she likely to develop significant systemic symptoms, and will she require urgent medical evaluation?
How would you manage these patients? Subscribe for evidence-based best practices and to discover the outcomes.
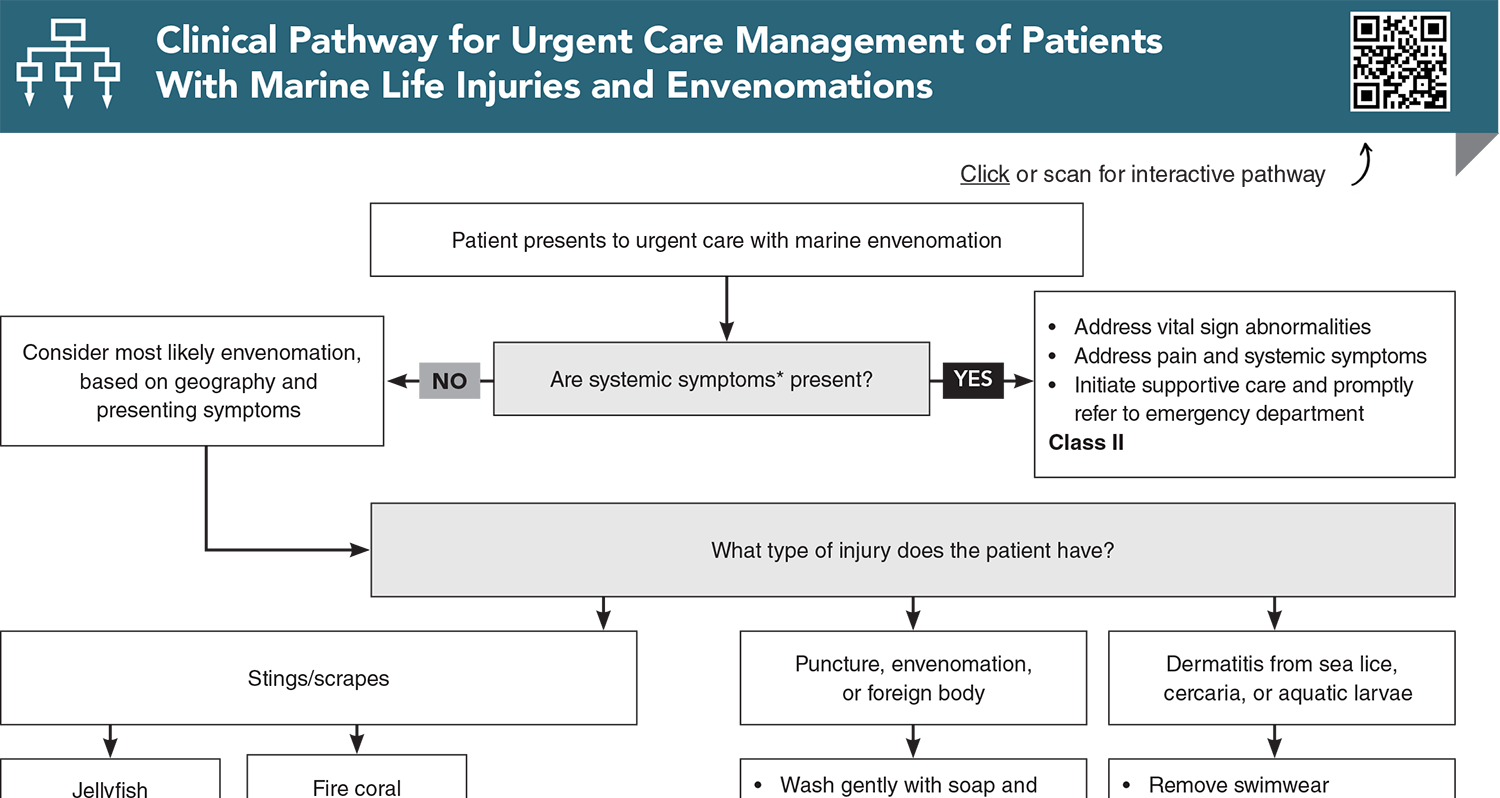
Clinical Pathway for Urgent Care Management of Patients With Marine Life Injuries and Envenomations
Subscribe to access the complete Clinical Pathway to guide your clinical decision making.
Buy this issue and
CME test to get 4 CME credits.
Key References
Following are the most informative references cited in this paper, as determined by the authors.
1. * Nickson CP, Waugh EB, Jacups SP, et al. Irukandji syndrome case series from Australia’s Tropical Northern Territory. Ann Emerg Med. 2009;54(3):395-403. (Case series from 1990 to 2007; 87 patients) DOI: 10.1016/j.annemergmed.2009.03.022
2. * Carrette TJ, Underwood AH, Seymour JE. Irukandji syndrome: a widely misunderstood and poorly researched tropical marine envenoming. Diving Hyperb Med. 2012;42(4):214-223. (Review) PMID: 23258458
7. * Davies E. “A deep dive into sea snakes, sea kraits and their aquatic adaptations.” Accessed February 15, 2026. (Website)
8. * Kapil S, Hendriksen S, Cooper JS. Cone snail toxicity. StatPearls. NCBI Bookshelf version: StatPearls Publishing; 2025. (Online book chapter)
16. * Loten C, Stokes B, Worsley D, et al. A randomised controlled trial of hot water (45˚ C) immersion versus ice packs for pain relief in bluebottle stings. Med J Aust. 2006;184(7):329-333. (Randomized controlled trial; 96 patients) DOI: 10.5694/j.1326-5377.2006.tb00265.x
18. * Baddour LM. Soft tissue infections following water exposure. UpToDate. 2025. Accessed February 15, 2026. (Research notes)
21. * Carrette TJ, Cullen P, Little M, et al. Temperature effects on box jellyfish venom: a possible treatment for envenomed patients? Med J Aust. 2002;177(11-12):654-655. (Animal model) DOI: 10.5694/j.1326-5377.2002.tb05000.x
27. * Welfare P, Little M, Pereira P, et al. An in-vitro examination of the effect of vinegar on discharged nematocysts of Chironex fleckeri. Diving Hyperb Med. 2014;44(1):30-34. (In-vitro study) PMID: 24687483
29. * Montgomery L, Seys J, Mees J. To pee, or not to pee: a review on envenomation and treatment in European jellyfish species. Mar Drugs. 2016;14(7). (Review) DOI: 10.3390/md14070127
Subscribe to get the full list of 30 references and see how the authors distilled all of the evidence into a concise, clinically relevant, practical resource.
Keywords: Marine injuries, marine envenomations, aquarium, jellyfish sting, box jellyfish, Irukandji syndrome, stingray, stingray injury, sea urchin, sea urchin spine, crown-of-thorns starfish, flower urchin, venomous fish, stonefish, lionfish, blue-ringed octopus, cone snail, siphonophore, sea snake, fire coral, seabather’s eruption, swimmer’s itch, cercarial dermatitis, sea lice, nematocyst, cnidarian, hot water immersion, thermolysis, venom, laceration, puncture, tissue necrosis, scrapes, tetanus prophylaxis, dermatitis, anaphylaxis, vinegar